Narrative review evaluating food contamination by endocrine disruptors present in food packaging.
Data sourceThe terms “endocrine disruptors” and “food packaging” were used in combination in the PubMed, MEDLINE and SciELO databases, evaluating studies, in humans, published in Portuguese, English, French and Spanish between 1990 and 2023.
Data synthesisPackaging, especially those made from plastic or recycled material, is an important source of food contamination by endocrine disruptors. Bisphenols and phthalates are the endocrine disruptors most frequently associated with food contamination from packaging. However, many unknown substances and even those legally authorized can cause harm to health when exposure is prolonged or when substances with additive effects are mixed. Furthermore, the discarding of packaging can cause contamination to continue into the environment.
ConclusionAlthough packaging materials are essential for the transport and storage of food, many of them are associated with chemical contamination. As it is not possible to exclude them from our routine, it is important to develop research aimed at identifying the endocrine disruptors present in them, including the effects of chronic exposure; and that regulatory agencies and industry come together to reduce or prevent this risk. Additionally, consumers must be instructed on how to purchase products, handle them and prepare them to reduce the migration of chemical substances into food.
Endocrine disruptors (ED) are exogenous agents that interfere with hormone synthesis, metabolism, and/or action. There is growing evidence of increasing exposure to these substances over the decades. Associated with this, an increase in the incidence and prevalence of diseases associated with ED1 has been observed. Some examples are hormonally mediated cancers, such as breast, prostate, and testicles, insulin resistance, metabolic syndrome, diabetes mellitus, obesity, allergies, autoimmune diseases, infertility and male genital malformations.2
Epidemiological studies that correlate ED with diseases must take into account that they are found ubiquitously in the air, water or soil.3 Therefore, it is possible that food can be contaminated at the different stages that precede its consumption, from obtaining (contamination of soil, rivers, oceans), handling, transportation, processing and production. Recently, contamination by chemical substances present in food packaging has been investigated.4 More than 10,000 chemicals are authorized in the United States to come into contact with food.5 Many of these substances, both intentionally and unintentionally added, have not been adequately tested for their ED effect. One of the factors responsible for the increase in exposure may be related to the increase in consumption of ultra-processed (UP) foods, due to changes in eating habits in recent decades. Fresh or minimally processed foods have been replaced by UP ones, which have been introduced earlier and earlier into children's diets. UP foods correspond to around 65 % of the daily energy consumption of a school-age child in the UK and USA.6 In Brazil, more specifically in the city of Pelotas, state of Rio Grande do Sul, data from the participants in the 1982, 1993 and 2004 cohorts demonstrated that UP food consumption was higher in younger cohorts (25.1 %, 29.8 %, and 33.7 % at ages 30, 22, and 11, respectively).7
Children constitute a particularly vulnerable group to exposure to these compounds due to higher relative consumption compared to adults, an immature clearance system, and longer exposure throughout life.8 This becomes evident when evaluating data from the National Health and Nutrition Examination Survey (NHANES) 2013–2014, which evaluated the 24-h dietary recall of children over six years of age, to correlate UP food intake with ED, including phthalates and bisphenols. For every 10 % increase in UP food consumption, there was an 8 % increase in the intake of chemical substances, with a stronger association in children and adolescents than in adults. Ultra-processed foods such as sandwiches, hamburgers, fries and ice cream were associated with higher concentrations of multiple chemicals.9
Although establishing causality between chronic exposure to chemical substances present in packaging and their adverse effect on human health is a difficult task, it is known that food packaging is an important source of exposure to ED, due to contamination of the packaging itself and the contamination of the environment after its disposal.2 Therefore, this article aims to describe the importance of food packaging and its role as a potential route of ED contamination, describe the ED most frequently found in food packaging, their adverse effects on the endocrine system, and recommend measures to prevent contamination by these agents.
Endocrine disruptorsAccording to the World Health Organization (WHO), ED are chemical substances present in the environment, whether natural or synthetic, which have the ability to mimic or interfere with the synthesis, secretion, transport, binding, action, or elimination of hormones, causing adverse effects on an organism, its offspring or (sub)populations. These substances can accumulate and persist in the environment causing long-term effects.10
Despite having a much lower affinity for the hormone receptor than the hormone itself, ED can have several mechanisms of action: agonistic effect, antagonistic effect, affecting the synthesis, transport, metabolism, binding to carrier proteins and excretion of hormones, altering the concentrations of natural hormones and inducing epigenetic modifications in hormone-producing or hormone-responsive cells. Through these mechanisms of action, they can interfere in the regulation of body growth and development, metabolism, reproduction, immunity, and behavior.10,11
Risk assessments have been historically conducted on an individual basis, but regulatory agencies have begun to consider the cumulative risk of mixing chemicals – the “cocktail effect”. Studies in pregnant animals with single exposure or binary mixtures of 7 and 10 ED with anti-androgenic action in microdoses confirmed that exposure to a single chemical did not induce or induce rare malformations, while mixtures caused malformations in around 50 % of males.12
Children, pregnant women, and workers in specific activities constitute the most vulnerable group to exposure to ED. There is growing evidence that exposure to ED during critical periods of embryological development can cause permanent changes in gene expression, a concept similar to that proposed by David Barker about intrauterine growth restriction influencing the prevalence of metabolic syndrome in adult life.13 This perhaps justifies the growing number of endocrinological diseases in childhood. However, it is worth remembering that long-term effects can be observed long after exposure and even have consequences for future generations.
The main EDs present in food packaging are described below.
Bisphenol ABisphenol A (BPA) is an additive that increases the flexibility and durability of plastics. Its exposure occurs orally or topically. BPA is often used in food packaging, for instance, to create epoxy resin for the inner lining of cans and kitchen utensils to minimize sulphuration and corrosion reactions. BPA is also used in the manufacturing of surface paints and printer inks, thermal bank cards or bill paper, medical and electronic equipment, toys, plastics and polymers used in the automobile industry, as well as in flame retardants and dental sealants. The use of BPA in the production of baby bottles, cups or dishes has been banned since 2011.1
BPA is an agonist of the estrogen receptor, glucocorticoid receptor, and peroxisome proliferator-activated receptor gamma (PPAR), interfering with the thyroid axis and androgen receptor (antiandrogenic action), inducing aromatase activity (promotes the conversion of androgens into estrogens), increasing serum levels of sex steroid binding globulin (SHBG), and reducing circulating levels of androstenedione and free testosterone.3,14
Exposure to BPA is frequent and widespread. Some reports from studies carried out in the USA, Germany and Canada show that more than 90 % of the individuals evaluated had measurable amounts of BPA in their urine.12 Exposure to BPA has been associated with an increase in cases of cryptorchidism, hypospadias, and reduced semen quality in men, suggesting a possible interference with male reproductive function.12
PhthalatesPhthalates are substances used in the manufacturing of plastics (plastic bottles, food packaging) and a wide range of products, such as adhesives, detergents and personal care products such as soaps, shampoos, cosmetics and nail polish. Because they have a weak bond with plastic polymers, they are easily released into the environment that surrounds them. One study evaluated the amount of phthalates in water from plastic bottles when they were distributed and after 45 days, under different storage conditions. The levels of a type of phthalate (DEHP) increased fourfold when exposed in some periods to temperatures of up to 40 °Celsius, such as when left in a car exposed to the sun. Even so, consumption levels remained well below those considered to be toxic. However, the authors recommend keeping PET bottles away from sun exposure and temperatures above 25 °Celsius.15
Its ED effect results from estrogenic and antiandrogenic action. A Chinese study compared 60 boys with constitutional delay in growth and puberty with 120 others with normal growth and puberty and found higher phthalate levels in the first group, as well as lower testosterone levels, suggesting that due to its antiandrogenic action, phthalate levels may play a role in constitutional delay in growth and puberty.16 A study in girls with precocious puberty (PP) evaluated levels of phthalate metabolites in 87 girls with PP and 63 control girls and applied a questionnaire on the forms of exposure. Girls with precocious puberty had significantly higher levels of a type of phthalate (DHT) than the controls. In response to the questionnaire, 65.1 % of girls with precocious puberty and 38 % of the control girls had regularly used some cosmetic products.17 Other studies correlate precocious puberty and phthalates, showing that the age at pubarche and thelarche seems to be inversely related to the quintiles of phthalate intake, that is, the higher the consumption, the earlier they occur.18 A study analyzing NHANES data from 2011 to 2016 on urinary phthalate levels and bone mineral density in 846 adolescents aged 12 to 19 years found a correlation between lower bone mass and higher urinary phthalate levels.19
PhytoestrogensPhytoestrogens are compounds with estrogenic action naturally produced by plants. Isoflavones, such as genistein, are found in soybeans, legumes and lentils. In 2012, the Avon Longitudinal Study of Parents and Children Cohort analyzed the type of milk consumed in early childhood, trying to find a correlation with age at menarche in 2920 Caucasian girls. In this study, consumption of soy formula before six months of age was associated with a slight reduction in the mean age at menarche, 12 years, and 4 months versus 12 years and 8 months in girls exposed to breastfeeding or non-soy formula.20
ParabensParabens have a similar action to phthalates and are often present concomitantly. They are widely used as preservatives in foods, cosmetics, and medications, due to their antimicrobial action, being easily absorbed by the human body. A cohort study of 337 children followed from birth to the peri‑pubertal period demonstrated that higher peri‑pubertal concentrations of methylparaben were associated with the anticipation of thelarche, pubarche and menarche in girls, while propylparaben was associated with precocious pubarche in girls and gonadarche in boys.21
BenzophenoneBenzophenone is a diethyl ketone, with estrogenic action, widely used as a food additive or in the paint of carton packaging and even in unpainted carton packaging if it was made from recycled paper.22 In animal studies, it has estrogenic and antiandrogenic effects, causing hypospadias in rats.22
OrganotinsOrganotins are used as antioxidants and stabilizers in plastic packaging and even glass, such as wine and beer bottles. These compounds may have androgenic action and bind with high affinity to the PPAR receptor and the retinoid X receptor, which play crucial roles in adipocyte differentiation and may be related to the obesity epidemic.22
AlkylphenolsAlkylphenols are organic compounds that persist for long periods in water and soil, bioaccumulating with their ED properties, especially estrogenic action. Pollution of the global water cycle with these remaining organic contaminants is one of the greatest challenges of our century.23
PerchloratesPerchlorates can interfere with the production of thyroid hormones. Perchlorate affects thyroid function by inhibiting the transport of iodine to the gland, which is essential for the production of T3 and T4. Exposure to this chemical, especially in pregnant women or infants with inadequate iodine intake, can compromise neurodevelopment.9
MelamineWith the recent awareness about the chemical components of plastics, substitutes for packaging and cutlery using bamboo and wood have been sought. However, due to a lack of regulation, sometimes these materials are not purely made of bamboo or wood and may contain substances known to be toxic, such as formaldehyde and melamine.24 Due to its high nitrogen content, melamine was added to formulas or dairy products to falsely increase their protein content, causing animal deaths due to its mixing in animal feed in 2007 in the USA and kidney disease in children in China due to its illegal addition to infant formulas. Since then, a series of studies have demonstrated that in smaller quantities melamine has potential ED effects on reproduction and anthropometric evolution.25
Food packagingFood packaging comprises materials used to package, wrap, protect and preserve food during storage, transportation and sale. These materials can be plastic, glass, paper, metal, wood and fabrics adapted to meet the specific characteristics of different types of food.26
They must comply with regulatory safety requirements, guarantee the integrity, quality and safety of food, in addition to providing nutritional information to consumers. Its main functions are5: (i) physical protection: protect against mechanical damage, impact, humidity, light and excessive temperature, as well as prevent the entry of water, air or microorganisms; (ii) preservation: help extend the shelf life of food, maintaining its freshness, flavor, texture and nutritional value for longer; (iii) information: information on the product's nutritional data, ingredients used, expiration date, instructions on storage and preparation and information on potential allergens (e.g., gluten); and (iv) brand identification: design and visual elements that identify the product, differentiating it from others on the market and influencing the consumer's purchasing decision.
Food packaging and contamination by endocrine disruptorsDespite these precautions, food packaging can be an important source of contamination by chemical substances used in its manufacture, which can potentially migrate into food. These substances can be those legally and intentionally added to packaging or those unintentionally added that occur from chemical reactions or degradation.27 Many of them have not been identified or sufficiently studied in relation to their ED effect. The risk of ED contamination is greater due to the fact that they are capable of causing adverse events even in small concentrations, making it difficult to establish an exposure threshold.2 Often, the duration of exposure for an adverse effect to be identified is prolonged, making longitudinal studies that show a causal relationship difficult. Another concern is the additive effect of mixing substances with similar action, meaning that the mixture can be toxic even if the concentration of its individual components is within the recommended limits.12 Aggregate exposure from other sources and previous contamination, before the food is placed inside the packaging, contribute to this difficulty. For instance, food contaminated at its origin with those exposed to pesticides in its agricultural cultivation, or fish contaminated by environmental pollutants.
The contamination of food by chemical substances and ED also varies according to the type of packaging used:
- -
Plastic packaging: most food packaging is made of plastic. BPA and phthalates are EDs used in the manufacture of plastic packaging such as bottles, plastic containers for storing food and PVC films.28 Contamination occurs when these EDs migrate from packaging materials to food, especially when there is heating, prolonged contact, repeated use of the packaging, or when the food is fatty or acidic.29
- -
Metal packaging: these packages, usually cans, are made of aluminum or steel, many internally coated with resins containing BPA to prevent corrosion and contamination of the food.8 However, BPA can migrate from the resin into the canned food, especially if the food is fatty or acidic.30
- -
Paper and cardboard packaging: these packaging may contain phthalates, paint residues, stickers, labels, glues and other chemicals with ED action that can contaminate the packaged food.31 Contamination is more likely to occur when using recycled paper and cardboard that uses chemical substances that are not recommended for food packaging.27
- -
Glass packaging: as glass is an inert material that does not release chemical substances, it is considered safe packaging for packaging food. However, glass containers may have sealing lids or internal linings made of plastic and metal can cause ED contamination.32
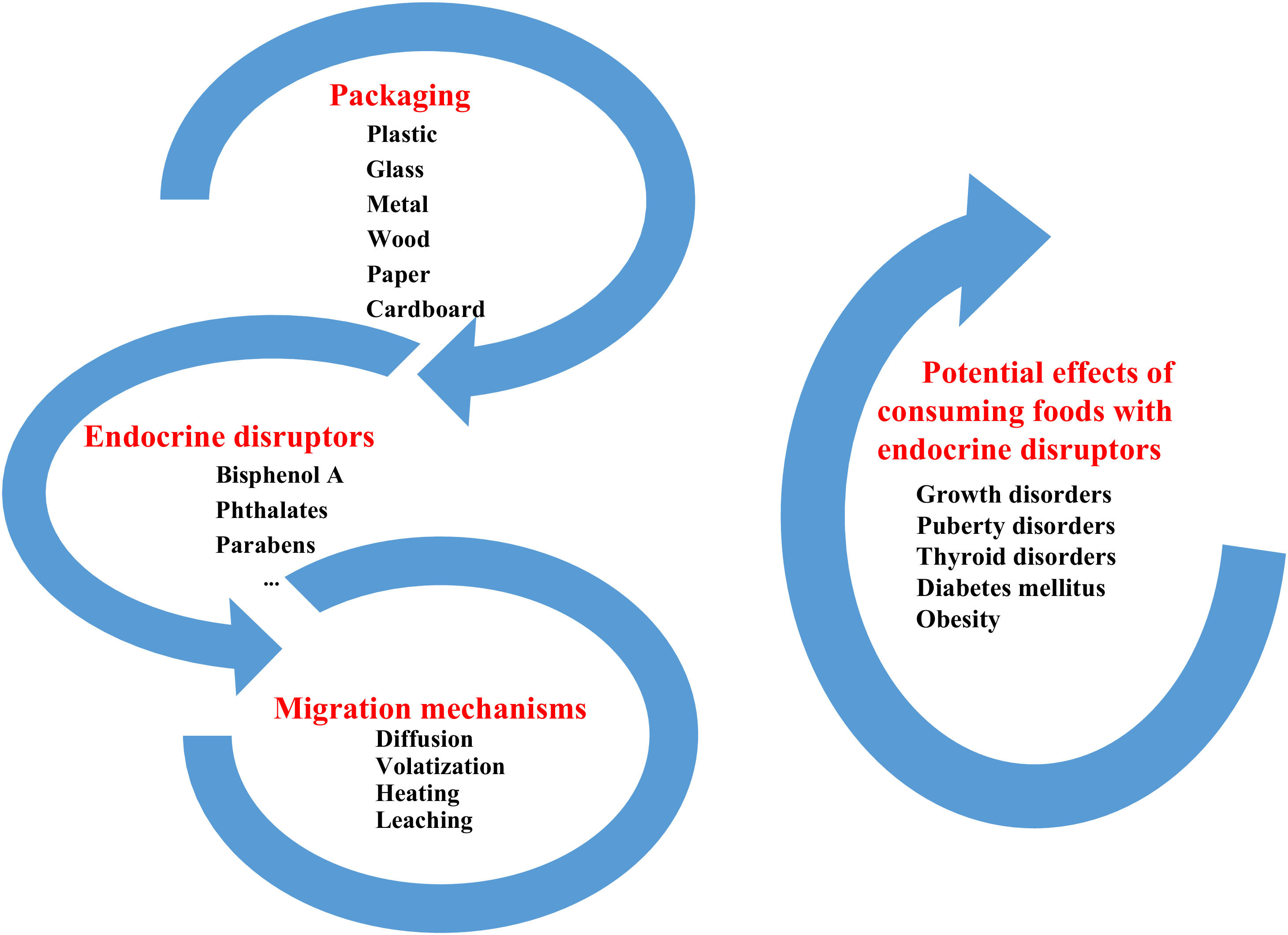
Figure 1 illustrates the food packaging cycle, ED, migration into food, consumption, and potential adverse effects.
Migration of endocrine disruptors from packaging into foodBefore being packaged, food can be contaminated at different stages, such as transportation (fuel exhaustion from vehicles, cross-contamination in transport used for other purposes), processing (contamination by disinfectants and cleaning products), production (water used, heating producing acrylamides and nitrosamines) and storage (exposure to naphthalenes).32
Because they are present in packaging, chemical substances, including ED, can migrate from packaging into food. This transfer depends on the chemical substance and its solubility, pH of the food (acidic, alkaline), whether the food is liquid or dry, fat content of the food, type of packaging, storage time and temperature or heating.26 Small packages, such as those intended for children, have a higher surface/volume ratio, therefore having a higher migration rate of chemical substances per kg of food22. The main mechanisms for ED migration from packaging to food are:33
- -
Direct contact: this is the most common form of migration when the ED comes into direct physical contact with the food.
- -
Diffusion: it occurs when the ED present in the packaging diffuses and enters the food. This mechanism is influenced by the difference in concentration, chemical characteristics of the substance, temperature and duration of contact.
- -
Leaching: leaching occurs when plastic chemicals are not firmly bonded to their polymer cores, breaking off and escaping into the food environment. Heating food in a microwave oven and prolonged contact between food and packaging increases leaching and the likelihood of contamination.
- -
Heating: the increase in temperature caused by heating accelerates the processes of migration and transfer of ED present in packaging to the food, by altering the structure of the chemical substance, facilitating contamination by molecules resulting from this metabolism.
- -
Volatilization: this contamination occurs when a substance converts into vapor or gas and disperses into the surrounding environment. In theory, it is possible that ED in food packaging could volatilize and disperse into the air near other foods, contaminating them.
Therefore, food contaminated by chemical substances present in the packaging is consumed daily, which has a greater impact on the most vulnerable groups such as children and pregnant women. Contamination continues in nature when the packaging is discarded. Although it is difficult or even impossible to prevent exposure to chemical substances present in food packaging, it is important to further study potential contaminants and how to avoid them.
Identification of endocrine disruptors transferred from packaging into foodTo test the migration of a chemical substance from packaging into food, global migration and specific migration are evaluated. In global migration, the total quantity of substances that migrate is assessed, without identifying which substances they are. In specific migration, the amount of migration of a given substance is specifically evaluated. These tests use food simulators, being carried out in a standardized way, under contact conditions of time and temperature similar to the actual contact conditions between the packaging material and the food. Testing the presence of ED in food cannot inform whether it came from the packaging, as there may have been previous contamination.
It is important that all chemical substances present in packaging are tested for their potential ED effects, including tests from low to high doses, avoiding extrapolating results from a single dose, and considering the additive effect caused by the mixture of substances.29
To detect the presence of ED in foods, several analytical methods are used, both chemical and biological tests. These techniques require obtaining a sample of the food, purifying it, and preparing it before the analysis to remove potential interferents. The main techniques used are:
- -
Gas chromatography with mass spectrometry (GC–MS): consists of the separation of compounds by gas chromatography, followed by their detection and identification using mass spectrometry. This method has high sensitivity and specificity, allowing the detection of very small amounts of ED present in the food.34
- -
Liquid chromatography with mass spectrometry (LC-MS): this method is used to evaluate the presence of polar and non-volatile ED in food matrices. It has excellent sensitivity and specificity to detect a wide variety of chemical compounds.35
- -
High-performance liquid chromatography (HPLC): a widely used method to quantify ED in foods. It can be coupled to ultraviolet, fluorescent and electrochemical detectors to assist in the identification and quantification of the ED under investigation.36
- -
Enzyme-linked immunosorbent assay (ELISA): it is based on the interaction between an antibody and the analyte being measured. Although it has a lower cost and is quick to test, it has low sensitivity and specificity compared to the two previously mentioned methods.37
- -
Biosensors: they use biological components, such as enzymes, antibodies or cells to detect and identify the presence of ED in food. They can be targeted to specific EDs, having good sensitivity and specificity.38
- -
Nuclear magnetic resonance with spectroscopy: a more expensive technique, which can be used to identify and quantify ED present in foods.39
There is increasing evidence that exposure to ED when it occurs during critical periods of embryological development, can cause permanent changes in gene expression programming. This perhaps explains the increasing numbers of endocrinological diseases in childhood, and the long-term effects can be felt long after the exposure.40 It should also be recalled that exposure to ED from food packaging is proportional to the volume of food in relation to the surface of the packaging and the volume ingested in relation to total body weight and that this relationship is greater in children.
Some specific activities also seem to be at greater risk. A case-control study compared the occupation of the parents of 73 boys with hypospadias with 146 control boys, chosen because they were the same age and came for consultation at the same clinic for minor illnesses. Children with hypospadias had twice as many fathers and five times as many mothers working in activities exposed to ED, such as farmers, hairdressers, painters or mechanics, suggesting that exposure to pesticides during preconception and prenatal life is associated with hypospadias and exposure to phthalates and alkylphenolic compounds are potentially risk factors.41
Community education and awareness about endocrine disruptors in food packagingThe main measure to reduce contact with ED is through regulation by public health and safety policies. Regulation has the potential to achieve a more far-reaching impact than recommendations that place all the onus on individuals to modify patterns of behavior and consumption.42
Pediatricians can contribute individually by raising awareness in families to identify ways through which children may be exposed to ED and help these parents find less toxic alternatives. The following strategies can be suggested to reduce exposure and contamination by endocrine disruptors (Table 1).43,44
Strategies to decrease contamination by endocrine disruptors.
It is evident from this narrative review that food packaging is a source of numerous chemical substances, several of which have documented ED effects on human health, especially when contact occurs during periods of greater vulnerability, such as during pregnancy or childhood or when it is systematic and in large proportions, as demonstrated in some groups of exposed workers.
A series of studies correlate exposure to ED and changes in childhood related to growth, development, puberty, weight and metabolism. Because they are correlation studies, they suggest, but cannot affirm, that these substances are triggering factors for these pathologies. However, when observing the increase in the prevalence of these endocrine diseases, the question arises as to which environmental factor may be contributing to this increase and what must be done to change this situation.
Everyone wants to enjoy the comfort and practicality of modern life, for instance, using packaged food, and everyone wants a “greener” and sustainable future. However, to reduce exposure to ED it is necessary to change one's lifestyle, habits and consumption patterns. These attitudes, in addition to reducing individual exposure, can also pressure commerce, industry and governments to improve public and private policies that will lead to the production of safer packaging.