this study aimed to evaluate the association of breakfast intake with cardiometabolic risk factors in a nationally-representative sample of Iranian pediatrics.
Methodsthe study participants considered of 5,625 school students aged 10-18 years, studied in the third survey of the national school-based surveillance system (CASPIAN-III). They were classified into three groups based on the number of days they ate breakfast: “regular breakfast eater” (6-7days/week), “often breakfast eater” (3-5days/week), and “seldom breakfast eater” (0-2 days/week). Metabolic syndrome (MetS) was defined based on the Adult Treatment Panel III (ATP III) criteria modified for the pediatric age group. Moreover, high total cholesterol, high low-density lipoprotein cholesterol (LDL-C) and generalized obesity were included as other cardiometabolic risk factors. Multiple logistic regression analyses were used to evaluate the association between the breakfast intake category and cardiometabolic risk factors.
Resultsthe number of subjects classified as “regular”, “often” and “seldom” breakfast eaters were 2,653(47.3%), 1,327(23.7%) and 1,624(29.0%), respectively. The average of triglycerides (TG), LDL-C, systolic blood pressure (SBP) and body mass index (BMI) were higher in the “seldom breakfast eater” group (P for trend<0.001), whereas the mean of high-density lipoprotein cholesterol (HDL-C) was lower in this group than their other counterparts. Seldom breakfast eaters had an increased risk of obesity, elevated TG and LDL-C, as well as low HDL-C compared to “regular breakfast eaters”. The risk of MetS was significantly increased in subjects who seldom ate breakfast (OR 1.96, 95% CI 1.18-3.27).
Conclusionsskipping breakfast is associated with increased risk of MetS and other cardiometabooic factors in children and adolescents. Promoting the benefit of eating breakfast could be a simple and important implication to prevent these risk factors.
O objetivo deste estudo foi avaliar a associação do consumo de café da manhã com fatores de risco cardiometabólico em uma amostra representativa, em termos nacionais, de pacientes de pediatria iranianos.
MétodosOs participantes do estudo, composto de 5.625 alunos em idade escolar de 10-18 anos, participaram da terceira pesquisa do sistema nacional de vigilância nas escolas (CASPIAN-III). Eles foram classificados em três grupos, com base na quantidade de dias em que consumiam café da manhã: “indivíduos que consomem café da manhã regularmente” (6-7 dias/semana), “indivíduos que consomem café da manhã normalmente” (3-5 dias/semana) e “indivíduos que consomem café da manhã raramente” (0-2 dias/semana). A síndrome metabólica (SM) foi definida com base nos critérios do III Painel de Tratamento de Adultos (ATP III), adaptados para a faixa etária pediátrica. Ademais, o colesterol total elevado, a lipoproteína de baixa densidade-colesterol elevada (LDL-C) e a obesidade generalizada foram incluídos como outros fatores de risco cardiometabólico. As análises de regressão logística múltipla foram utilizadas para avaliar a associação entre a categoria consumo de café da manhã e fatores de risco cardiometabólico.
ResultadosA quantidade de pessoas classificadas como indivíduos que consomem café da manhã “regularmente”, “normalmente” e “raramente” foram 2.653 (47,3%), 1.327 (23,7%) e 1.624 (29%), respectivamente. As médias de triglicerídeos (TG), LDL-C, pressão arterial sistólica (PAS) e índice de massa corporal (IMC) foram mais elevadas no grupo de “indivíduos que consomem café da manhã raramente” (P para tendência < 0,001), ao passo que a lipoproteína de alta densidade-colesterol (HDL-C) foi menor nesse grupo que nos outros. Os indivíduos que consomem café da manhã raramente apresentaram um aumento no risco de obesidade, TG e LDL-C elevados, bem como baixo HDL-C em comparação a “indivíduos que consomem café da manhã regularmente”. O risco de SM foi significativamente maior nos indivíduos que consomem café da manhã raramente (RC 1,96, 95% IC 1,18-3,27).
ConclusõesPular o café da manhã está relacionado a aumento no risco de SM e outros fatores cardiometabólicos em crianças e adolescentes. Promover o benefício do consumo do café da manhã pode ser uma implicação simples e importante para evitar esses fatores de risco.
Chronic diseases have emerged as a rapidly increasing public health problem in developing countries.1 Interest in childhood precursors to chronic diseases, particularly cardiovascular disease (CVD), is increasing because both behavioral and biological risk factors of such diseases persist from childhood into adulthood, and the several cardiometabolic risk factors, including obesity, dyslipidemia and metabolic syndrome (MetS), are followed from childhood to adult life and diseases.2,3
Some behavioral variables, including physical inactivity, unhealthy dietary habits, smoking and skipping meals, mainly breakfast, are associated with the development of CVD in later life.4
Breakfast is an important consumption for maintaining adequate intake and health for children and adolescents.5 It is estimated that children consume about twenty percent of their daily energy intake at breakfast.6 Breakfast consumption has been associated with intake of most vitamins and minerals and improved diet quality in children and adolescents.7 One dietary pattern that has an important role in maintaining normal weight in children and adolescence is the consumption of breakfast.8 Some studies have reported a lower risk of overweight and obesity among children having breakfast regularly compared with those frequently skip it.9,10 Research reveals that not only is breakfast consumption important, but also that the frequency of breakfast may be an important factor influencing weight.11
Similar to many other developing countries, the epidemiologic transition along with rapid lifestyle changes has made Iranian children prone to cardiometabolic risk factors, and, as a result, to chronic diseases in adulthood.12,13 Consequently, for the first time in Iran, we determined the association of breakfast pattern with cardiometabolic risk factors in a large nationally-representative sample of children and adolescents.
Materials and methodsThe data used in this study was obtained as a part of the third survey of the school-based surveillance system entitled “Childhood and Adolescence Surveillance and Prevention of Adult Noncommunicable Disease” (CASPIAN) study. The school-based nationwide health survey was conducted to assess nationally-representative high risk behaviors in school students in Iran (2009–2010). We have previously described the methods of this study in details.14
The present study was performed among 5,625 students aged 10-18 years who were selected via multistage random cluster sampling method from urban and rural areas of 27 provinces in Iran. Eligible schools in our study were stratified according to the information bank of the Ministry of Health and Medical Education and then they were selected randomly. In selected schools, the students were also selected randomly. Sampling and examinations were begun after complete explanation of the study's objectives and protocols for students and their parents, obtaining the written informed consent from parents and also the oral assent from the students. A team of trained health care professionals recorded information in a checklist and carried out the examinations under the standard protocol by using calibrated instruments. The study was approved by the Ethical Committee and other relevant national regulatory organizations.
Clinical and laboratory measurementsTrained research assistants measured the adolescents’ height and weight according to standardized protocols. Weight was recorded in light clothing to the nearest 0.1kg on a SECA digital weighing scale (SECA, Germany) and height was measured without shoes to the nearest 0.1cm. Body mass index (BMI) was calculated from weight and height BMI=weight (kg)/height (m2).Waist circumference (WC) was measured using a non-elastic tape to the nearest 0.1cm over skin, midway between the iliac crest and the lowest rib in standing position.
Two measurements of systolic blood pressure (SBP) and diastolic blood pressure (DBP) were performed using a standardized mercury sphygmomanometer on the right arm after a 15-minute rest in a sitting position; the first and fifth Korotkoff sounds were recorded as systolic and diastolic BP, respectively. The mean of the two measurements was considered as the subject's blood pressure.
A venous blood sample was drawn from all the study participants after 12hours of overnight fasting and delivered to the laboratory on the same day. Fasting blood glucose (FBG), total cholesterol (TC), high density lipoprotein-cholesterol (HDL-C), low-density lipoprotein cholesterol (LDL-C), and triglycerides (TG) were measured enzymatically by auto-analyzers. HDL-C was determined after dextran sulfate-magnesium chloride precipitation of non-HDL-C.15 LDL- C was calculated in serum samples with TG ≤ 400mg/dl according to the Friedewald equation.16 Considering that collecting the highest quality data was critical to the success of our multi-center project, the Data and Safety Monitoring Board (DSMB) of the project took into account the different levels of quality assurance and control.
Demographic information was completed by obtaining data for all officially enrolled students in the sampled classes from the school record. Family based characteristics (family history of chronic diseases hypertension,dyslipidemia,diabetes,and obesity, parental level of education, possessing a family private car and type of home), dietary behaviors, physical activity, and sedentary lifestyle were assessed by an interview carried out with parents or child by a trained researcher.
Parental education level was based on the parent with the highest total years of schooling. In this study, information regarding breakfast a child had in the past week was collected. Parents reported, on a Likert scale questionnaire, the weekly frequency (none, 1-2 days, 3-6 days, every day) of breakfast eating at home. For statistical analysis, each weekly frequency received a name (0-2 days per week [Seldom]; 3-5 days per week [Often]; 6-7 days [Regular]). To evaluate the physical activity by using principal components analysis (PCA), two indicators were used including: (i) hours of physical education at school or outside the school (at least thirty minutes per day); and, (ii) hours of sedentary lifestyle (included: watching television and working on the computer) at home.
Definition of termsSubjects were classified as having MetS if they had at least three of the following criteria according to Adult Treatment Panel III (ATP III) criteria modified for the pediatric age group.17 abdominal obesity–WC at or above the 90th percentile value for age and sex; elevated BP–either systolic or diastolic BP at or above the 90th percentile for age, sex and height; low HDL-C–HDL-C ≤ 40(< 50) mg/dL (except in boys of 15-19 years old in which the cut off was < 45mg/dL); high TG: TG ≥ 100mg/dL) was taken as the 90th percentile value for age; high FBG–FBG levels of ≥100mg/dL.
Three main parameters of high total cholesterol, high LDL-C and general obesity were included in this study as other cardiometabolic risk factors. High cholesterol and low-density lipoprotein cholesterol were defined according to the recent recommendations by the American Heart Association; i.e. total cholesterol ≥ 200mg/dL, LDL-C>110mg/dlL.18 The definition of generalized obesity was considered as BMI > 95th percentile. Abdominal obesity was defined as waist to height ratio (WHtR) more than 0.5.19
Statistical analysisMeans ± SD were used to express standard descriptive statistics. Categorical variables were expressed as percentages. Differences among means were investigated by T-test and ANOVA. Comparison of percentages of the categorized variables was made using the Pearson Chi-square test. Logistic regression analyses were used to evaluate the association between the breakfast intake category and cardiometabolic risk factors in each model as possible confounders. All statistical analyses were performed using programs available in the SPSS version 16.0 statistical package for Windows (SPSS Inc., Chicago, Illinois). p < 0.05 was considered as statistically significant.
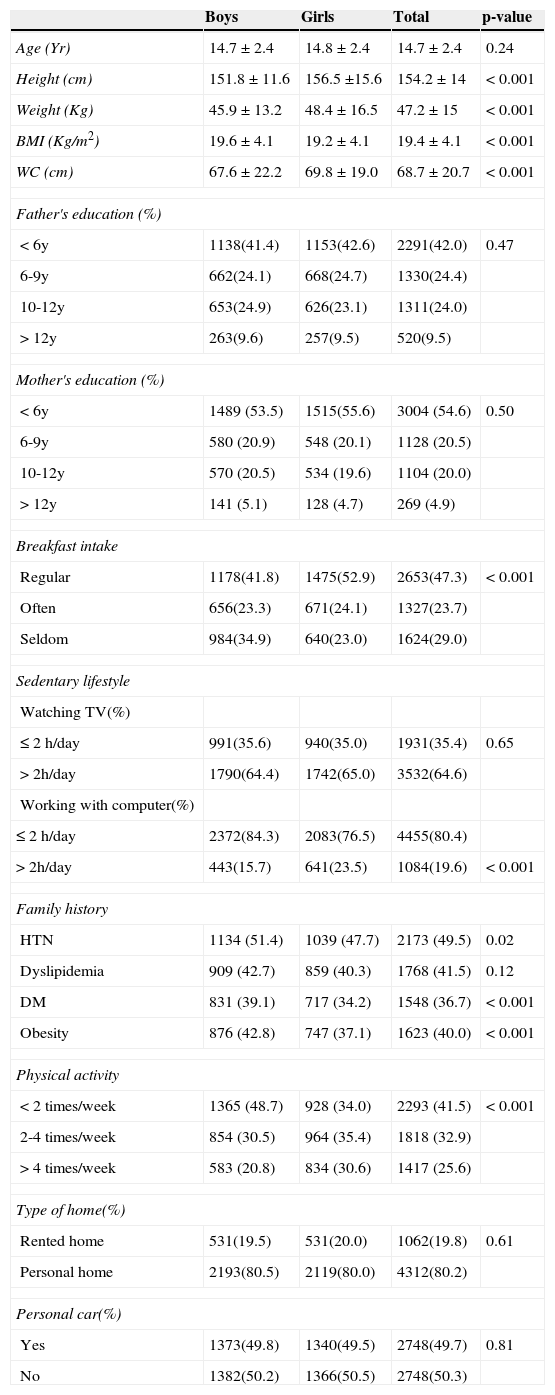
ResultsThe participants of this multicenter study included 5,604 students aged 10-18 years. The anthropometric and other characteristics of the individuals who were eligible for this study are stratified by sex and are shown in Table 1. Compared with boys, girls had significantly higher heights, weights, BMIs and WCs.
Characteristics of participants according to the sex: the CASPIAN-III Study.
| Boys | Girls | Total | p-value | |
|---|---|---|---|---|
| Age (Yr) | 14.7 ± 2.4 | 14.8 ± 2.4 | 14.7 ± 2.4 | 0.24 |
| Height (cm) | 151.8 ± 11.6 | 156.5 ±15.6 | 154.2 ± 14 | < 0.001 |
| Weight (Kg) | 45.9 ± 13.2 | 48.4 ± 16.5 | 47.2 ± 15 | < 0.001 |
| BMI (Kg/m2) | 19.6 ± 4.1 | 19.2 ± 4.1 | 19.4 ± 4.1 | < 0.001 |
| WC (cm) | 67.6 ± 22.2 | 69.8 ± 19.0 | 68.7 ± 20.7 | < 0.001 |
| Father's education (%) | ||||
| < 6y | 1138(41.4) | 1153(42.6) | 2291(42.0) | 0.47 |
| 6-9y | 662(24.1) | 668(24.7) | 1330(24.4) | |
| 10-12y | 653(24.9) | 626(23.1) | 1311(24.0) | |
| > 12y | 263(9.6) | 257(9.5) | 520(9.5) | |
| Mother's education (%) | ||||
| < 6y | 1489 (53.5) | 1515(55.6) | 3004 (54.6) | 0.50 |
| 6-9y | 580 (20.9) | 548 (20.1) | 1128 (20.5) | |
| 10-12y | 570 (20.5) | 534 (19.6) | 1104 (20.0) | |
| > 12y | 141 (5.1) | 128 (4.7) | 269 (4.9) | |
| Breakfast intake | ||||
| Regular | 1178(41.8) | 1475(52.9) | 2653(47.3) | < 0.001 |
| Often | 656(23.3) | 671(24.1) | 1327(23.7) | |
| Seldom | 984(34.9) | 640(23.0) | 1624(29.0) | |
| Sedentary lifestyle | ||||
| Watching TV(%) | ||||
| ≤ 2 h/day | 991(35.6) | 940(35.0) | 1931(35.4) | 0.65 |
| > 2h/day | 1790(64.4) | 1742(65.0) | 3532(64.6) | |
| Working with computer(%) | ||||
| ≤ 2 h/day | 2372(84.3) | 2083(76.5) | 4455(80.4) | |
| > 2h/day | 443(15.7) | 641(23.5) | 1084(19.6) | < 0.001 |
| Family history | ||||
| HTN | 1134 (51.4) | 1039 (47.7) | 2173 (49.5) | 0.02 |
| Dyslipidemia | 909 (42.7) | 859 (40.3) | 1768 (41.5) | 0.12 |
| DM | 831 (39.1) | 717 (34.2) | 1548 (36.7) | < 0.001 |
| Obesity | 876 (42.8) | 747 (37.1) | 1623 (40.0) | < 0.001 |
| Physical activity | ||||
| < 2 times/week | 1365 (48.7) | 928 (34.0) | 2293 (41.5) | < 0.001 |
| 2-4 times/week | 854 (30.5) | 964 (35.4) | 1818 (32.9) | |
| > 4 times/week | 583 (20.8) | 834 (30.6) | 1417 (25.6) | |
| Type of home(%) | ||||
| Rented home | 531(19.5) | 531(20.0) | 1062(19.8) | 0.61 |
| Personal home | 2193(80.5) | 2119(80.0) | 4312(80.2) | |
| Personal car(%) | ||||
| Yes | 1373(49.8) | 1340(49.5) | 2748(49.7) | 0.81 |
| No | 1382(50.2) | 1366(50.5) | 2748(50.3) | |
BMI, body mass index; WC, waist circumference; HTN, hypertension; DM, diabetes mellitus.
Data are means (SD) unless indicated otherwise. p < 0.05 is significant.
The number of subjects classified as “usually”,“often” and “seldom” breakfast eaters were 2,653 (47.3%), 1,327 (23.7%) and 1,624 (29.0%), respectively. Eating breakfast daily was identified in more than 50% of girls, whereas 34.9% of boys seldom ate breakfast.
Among girls, 30.6% reported physical activity more than 4 times per week, whereas 20.8% of boys met this criterion.
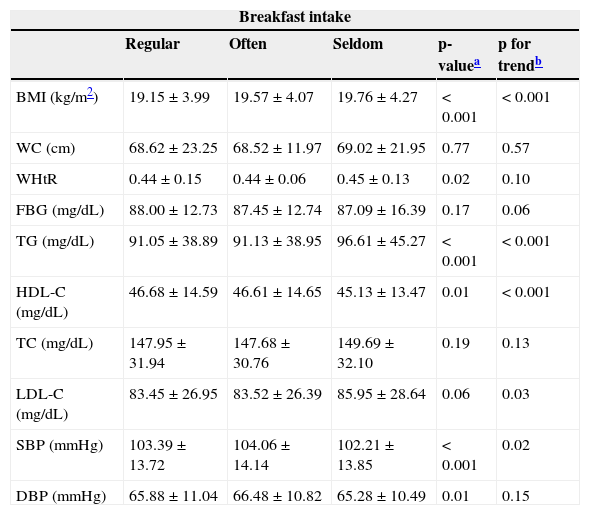
Mean values of various cardiometabolic risk factors according to the breakfast consumption group are presented in Table 2. The average of TG, LDL-C, SBP and BMI was significantly higher in the “seldom breakfast eater” group than in the “usual breakfast eater” group (p for trend < 0.01), whereas the mean of HDL-C was significantly lower in this group than its other counterparts. No significant difference in FBS, TC, and WC was found among the three breakfast consumption groups.
Cardiometabolic values in children and adolescents by breakfast consumption.
| Breakfast intake | |||||
|---|---|---|---|---|---|
| Regular | Often | Seldom | p-valuea | p for trendb | |
| BMI (kg/m2) | 19.15 ± 3.99 | 19.57 ± 4.07 | 19.76 ± 4.27 | < 0.001 | < 0.001 |
| WC (cm) | 68.62 ± 23.25 | 68.52 ± 11.97 | 69.02 ± 21.95 | 0.77 | 0.57 |
| WHtR | 0.44 ± 0.15 | 0.44 ± 0.06 | 0.45 ± 0.13 | 0.02 | 0.10 |
| FBG (mg/dL) | 88.00 ± 12.73 | 87.45 ± 12.74 | 87.09 ± 16.39 | 0.17 | 0.06 |
| TG (mg/dL) | 91.05 ± 38.89 | 91.13 ± 38.95 | 96.61 ± 45.27 | < 0.001 | < 0.001 |
| HDL-C (mg/dL) | 46.68 ± 14.59 | 46.61 ± 14.65 | 45.13 ± 13.47 | 0.01 | < 0.001 |
| TC (mg/dL) | 147.95 ± 31.94 | 147.68 ± 30.76 | 149.69 ± 32.10 | 0.19 | 0.13 |
| LDL-C (mg/dL) | 83.45 ± 26.95 | 83.52 ± 26.39 | 85.95 ± 28.64 | 0.06 | 0.03 |
| SBP (mmHg) | 103.39 ± 13.72 | 104.06 ± 14.14 | 102.21 ± 13.85 | < 0.001 | 0.02 |
| DBP (mmHg) | 65.88 ± 11.04 | 66.48 ± 10.82 | 65.28 ± 10.49 | 0.01 | 0.15 |
BMI, body mass index; WC, waist circumference; WHtR, waist to height ratio; FBG, fasting blood glucose; TG, triglycerides; HDL-C, high-density lipoprotein-cholesterol; TC, total cholesterol; LDL-C, low-density lipoprotein cholesterol; SBP, systolic blood pressure; DBP, diastolic blood pressure; SD, standard deviation.
All values are means ± SDs.
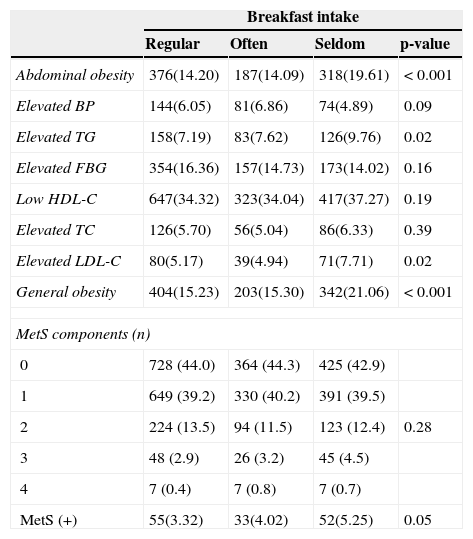
Table 3 illustrates the prevalence of the various cardiometabolic risk factors according to the breakfast eating category. It was observed that the “seldom breakfast eater” group had the highest prevalence of subjects with abdominal obesity, elevated TG, elevated LDL-C and general obesity compared with the other two groups. Abdominal obesity was present in 19.6% of the “seldom breakfast eater” group vs. the other two groups (p < 0.001), similarly for elevated TG (9.8%; p = 0.02), elevated LDL-C (7.7%; p = 0.02) and general obesity (21.1%; p < 0.001). “Seldom breakfast eaters” were significantly more likely to present metabolic syndrome (MetS) than those having breakfast (p = 0. 05).
Prevalence of cardiometabolic risk factors according to breakfast intake categories.
| Breakfast intake | ||||
|---|---|---|---|---|
| Regular | Often | Seldom | p-value | |
| Abdominal obesity | 376(14.20) | 187(14.09) | 318(19.61) | < 0.001 |
| Elevated BP | 144(6.05) | 81(6.86) | 74(4.89) | 0.09 |
| Elevated TG | 158(7.19) | 83(7.62) | 126(9.76) | 0.02 |
| Elevated FBG | 354(16.36) | 157(14.73) | 173(14.02) | 0.16 |
| Low HDL-C | 647(34.32) | 323(34.04) | 417(37.27) | 0.19 |
| Elevated TC | 126(5.70) | 56(5.04) | 86(6.33) | 0.39 |
| Elevated LDL-C | 80(5.17) | 39(4.94) | 71(7.71) | 0.02 |
| General obesity | 404(15.23) | 203(15.30) | 342(21.06) | < 0.001 |
| MetS components (n) | ||||
| 0 | 728 (44.0) | 364 (44.3) | 425 (42.9) | |
| 1 | 649 (39.2) | 330 (40.2) | 391 (39.5) | |
| 2 | 224 (13.5) | 94 (11.5) | 123 (12.4) | 0.28 |
| 3 | 48 (2.9) | 26 (3.2) | 45 (4.5) | |
| 4 | 7 (0.4) | 7 (0.8) | 7 (0.7) | |
| MetS (+) | 55(3.32) | 33(4.02) | 52(5.25) | 0.05 |
BP, blood pressure; TG, triglycerides; FBG, fasting blood glucose; HDL-C, high-density lipoprotein-cholesterol; TC, total cholesterol; LDL-C, low-density lipoprotein cholesterol; MetS, metabolic syndrome.
Data are N (percentage).
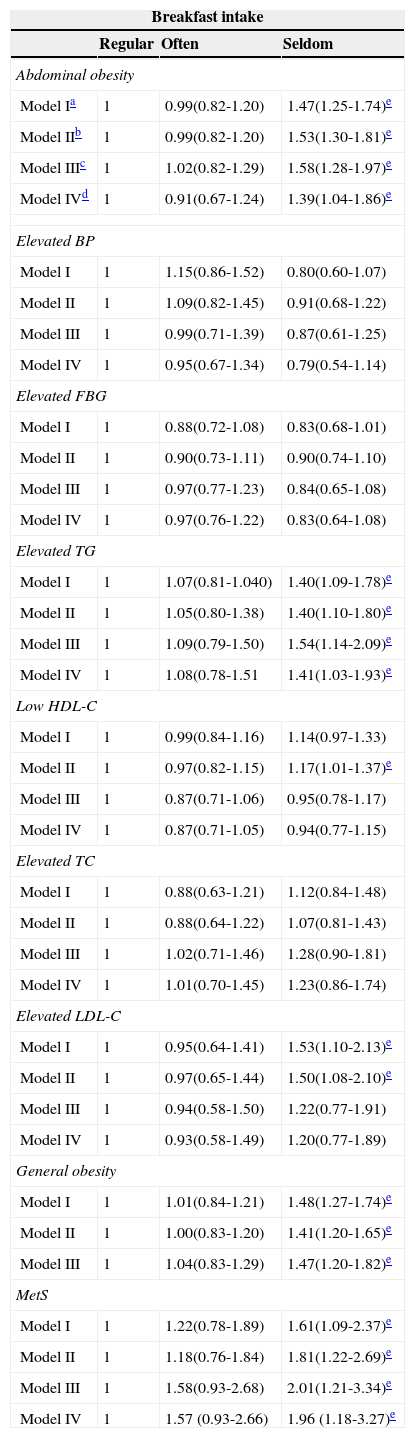
The odds ratios for risk of cardiometabolic factors across breakfast intake categories are shown in Table 4. As it is presented in this Table, “seldom breakfast eaters” were found to have the increased risk of abdominal obesity from 39% to 58% in all the models compared to the usual breakfast eater. In addition, in the model adjusting for age and sex, the risk of elevated LDL-C and low HDL-C increased in the children who seldom ate breakfast. In the multivariate model (Model IV), those who seldom ate breakfast had a significantly higher risk of elevated TG (OR 1.41, 95% CI 1.03-1.93), general obesity (OR 1.47, 95% CI 1.20-1.82), abdominal obesity (OR 1.39, 95% CI 1.04-1.86), and MetS (OR 1.96, 95% CI 1.18-3.27).
Odd ratios (95% CI) for cardiometabolic risk factors and pattern of breakfast intake.
| Breakfast intake | |||
|---|---|---|---|
| Regular | Often | Seldom | |
| Abdominal obesity | |||
| Model Ia | 1 | 0.99(0.82-1.20) | 1.47(1.25-1.74)e |
| Model IIb | 1 | 0.99(0.82-1.20) | 1.53(1.30-1.81)e |
| Model IIIc | 1 | 1.02(0.82-1.29) | 1.58(1.28-1.97)e |
| Model IVd | 1 | 0.91(0.67-1.24) | 1.39(1.04-1.86)e |
| Elevated BP | |||
| Model I | 1 | 1.15(0.86-1.52) | 0.80(0.60-1.07) |
| Model II | 1 | 1.09(0.82-1.45) | 0.91(0.68-1.22) |
| Model III | 1 | 0.99(0.71-1.39) | 0.87(0.61-1.25) |
| Model IV | 1 | 0.95(0.67-1.34) | 0.79(0.54-1.14) |
| Elevated FBG | |||
| Model I | 1 | 0.88(0.72-1.08) | 0.83(0.68-1.01) |
| Model II | 1 | 0.90(0.73-1.11) | 0.90(0.74-1.10) |
| Model III | 1 | 0.97(0.77-1.23) | 0.84(0.65-1.08) |
| Model IV | 1 | 0.97(0.76-1.22) | 0.83(0.64-1.08) |
| Elevated TG | |||
| Model I | 1 | 1.07(0.81-1.040) | 1.40(1.09-1.78)e |
| Model II | 1 | 1.05(0.80-1.38) | 1.40(1.10-1.80)e |
| Model III | 1 | 1.09(0.79-1.50) | 1.54(1.14-2.09)e |
| Model IV | 1 | 1.08(0.78-1.51 | 1.41(1.03-1.93)e |
| Low HDL-C | |||
| Model I | 1 | 0.99(0.84-1.16) | 1.14(0.97-1.33) |
| Model II | 1 | 0.97(0.82-1.15) | 1.17(1.01-1.37)e |
| Model III | 1 | 0.87(0.71-1.06) | 0.95(0.78-1.17) |
| Model IV | 1 | 0.87(0.71-1.05) | 0.94(0.77-1.15) |
| Elevated TC | |||
| Model I | 1 | 0.88(0.63-1.21) | 1.12(0.84-1.48) |
| Model II | 1 | 0.88(0.64-1.22) | 1.07(0.81-1.43) |
| Model III | 1 | 1.02(0.71-1.46) | 1.28(0.90-1.81) |
| Model IV | 1 | 1.01(0.70-1.45) | 1.23(0.86-1.74) |
| Elevated LDL-C | |||
| Model I | 1 | 0.95(0.64-1.41) | 1.53(1.10-2.13)e |
| Model II | 1 | 0.97(0.65-1.44) | 1.50(1.08-2.10)e |
| Model III | 1 | 0.94(0.58-1.50) | 1.22(0.77-1.91) |
| Model IV | 1 | 0.93(0.58-1.49) | 1.20(0.77-1.89) |
| General obesity | |||
| Model I | 1 | 1.01(0.84-1.21) | 1.48(1.27-1.74)e |
| Model II | 1 | 1.00(0.83-1.20) | 1.41(1.20-1.65)e |
| Model III | 1 | 1.04(0.83-1.29) | 1.47(1.20-1.82)e |
| MetS | |||
| Model I | 1 | 1.22(0.78-1.89) | 1.61(1.09-2.37)e |
| Model II | 1 | 1.18(0.76-1.84) | 1.81(1.22-2.69)e |
| Model III | 1 | 1.58(0.93-2.68) | 2.01(1.21-3.34)e |
| Model IV | 1 | 1.57 (0.93-2.66) | 1.96 (1.18-3.27)e |
CI, confidence interval; BP, blood pressure; TG, triglycerides; FBG, fasting blood glucose; HDL-C, high-density lipoprotein-cholesterol; TC, total cholesterol; LDL-C, low-density lipoprotein cholesterol; MetS, metabolic syndrome.
This study confirmed the association between breakfast frequency and CVD risk factors in a nationally-representative sample of Iranian children and adolescents. We found skipping breakfast increased the risk of general and abdominal obesity, MetS and having elevated TG, LDL-C and lower HDL-C in the children.
Previous studies reported that skipping breakfast is a behavioral factor related to the development of obesity.20,21 In the present study, we observed a significant association between seldom eating breakfast and general and abdominal obesity. When other factors were added to the model, this association remained or was only slightly weakened. Che et al. reported that seldom breakfast eaters had a lower total energy intake but a higher BMI than did breakfast eaters.11 Another study reported that the usual breakfast eater consumed greater amounts of energy, carbohydrates, and fiber but lower total percentages of total calories from fat.10 Those who daily eat breakfast also seem much more physically active than breakfast skippers. This dietary profile has the potential to improve energy balance and may improve glucose and insulin parameters and lead to increased satiety and lower weight.22 These results suggest that although skipping breakfast results in a lower daily energy intake, it increases eating snacks, sedentary lifestyle and cannot be used to control obesity.23 In contrast, eating breakfast is associated with increased eating frequency and this may in turn promote less efficient energy utilization by increasing dietary-induced thermogenesis, leading to a lower BMI.24
A complex interaction of environment and behavioral factors is suggested as the underlying causes of MetS. However, the impact of diet pattern on this health problem is inconclusive.25 We found that skipping breakfast significantly increased the risk of having MetS and cardiovascular risk factors. Our findings are in line with the results of a study among Australian children that showed that skipping breakfast may have determined the effects on their cardiometabolic health.26
Our findings regarding cardiovascular risk factors are supported by the result of a clinical trial. In that study, Farshchi et al. found women had higher total cholesterol and LDL-C after skipping breakfast than the ones who ate breakfast.27 Another study showed that weekly frequency of eating breakfast was negatively associated with fasting glucose and triglycerides regardless of other variables.26 As indicated in the current study, the risk of elevated TG, LDL-C and low HDL-C was significantly increased in subjects who skipped breakfast. Population-based studies in the Middle East have shown a markedly high prevalence of dyslipidemia in this region.28 This can be explained by an ethnic predisposition to MetS in Iran and its neighbouring countries.29 In addition, the changes in lipid levels may be due to change in dietary habits which have led to a considerable imbalance in food consumption, with low nutrient density characterizing diets among more than a third of the households.30 On the other hand, one of the most important changes in lifestyle is skipping meals, mainly breakfast. It has been reported to be associated with unhealthy behaviors, such as consumption of a poorer diet, and having physical inactivity10 that can result in higher MetS components.31 In prevention and treatment of MetS, we might benefit more from regular healthy meals than from skipping meals. Because common breakfast comes from the core food groups, it is a nutritious meal and is low in fat.32 So, for compensation later during the day, breakfast skippers have higher intakes of fat, energy, and lower intakes of fiber, vitamins and minerals than breakfast eaters.33 Interestingly, in our study, the MetS components that were more strongly related to skipping breakfast were waist circumference, TG and low HDL-C, which are the well-known predictors of insulin resistance, and CVD risk, so emphasizing the importance of eating breakfast as a possible behavioral pattern for cardiometabolic risk, especially MetS.31
Our study has several limitations. First, we used the cross-sectional nature of the study, which does not allow a causal relationship between breakfast consumption and cardiometabolic risk factors to be confirmed. Second, cardiovascular risk factors are heterogeneous and other factors such as hereditary factors, nutrition intake, and type of breakfast must be considered. Given that we could not assess the pubertal stage in such a large population, the influences of puberty on CVD risk is therefore another limitation of the present study.
The strength of this study includes the large national sample size. We had measures of socioeconomic and lifestyle factors that we were able to include in our models to reduce possible confounding. To our knowledge, this is the first study in Iran to examine associations of breakfast consumption with MetS and cardiovascular risk factors in children and adolescents. Future cohort studies using a prospective design could evaluate these findings and investigate potential mechanisms.
In conclusion, Skipping breakfast is a common behavior among Iranian children and adolescents, and is associated with increased risk of MetS and other cardiovascular factors. Improvement of habits related to the frequency of breakfast consumption, in this age range, could be a useful and important implication to prevent these risk factors.
Conflicts of interestThe authors declare no conflicts of interest.
This nationwide survey was conducted in Iran with the cooperation of the Ministry of Health and Medical Education; Ministry of Education and Training, Child Growth and Development Research Center, Isfahan University of Medical Sciences; and Endocrinology and Metabolism Research center of Tehran University of Medical Sciences.
Please cite this article as: Shafiee G, Kelishadi R, Qorbani M, Motlagh ME, Taheri M, Ardalan G, et al. Association of breakfast intake with cardiometabolic risk factors. J Pediatr (Rio J). 2013;89:575–582.