To evaluate the association between dietary patterns and cardiometabolic risk factors in children and adolescents.
Data sourceThis article followed the recommendations of PRISMA, which aims to guide review publications in the health area. The article search strategy included searches in the electronic databases MEDLINE via PubMed, Scopus, and LILACS. There was no date limitation for publications. The descriptors were used in English according to MeSH and in Portuguese according to DeCS. Only articles on dietary patterns extracted by the a posteriori methodology were included. The question to be answered was: how much can an “unhealthy” dietary pattern influence biochemical and inflammatory markers in this population?
Data synthesisThe studies showed an association between dietary patterns and cardiometabolic alterations. The patterns were characterized as unhealthy when associated to the consumption of ultraprocessed products, poor in fiber and rich in sodium, fat, and refined carbohydrates. Despite the associations, in several studies, the strength of this association for some risk markers was reduced or lost after adjusting for confounding variables.
ConclusionThere was a positive association between “unhealthy” dietary patterns and cardiometabolic alterations in children and adolescents. Some unconfirmed associations may be related to the difficulty of assessing food consumption. Nevertheless, studies involving dietary patterns and their association with risk factors should be performed in children and adolescents, aiming at interventions and early changes in dietary habits considered to be inadequate.
Avaliar a associação encontrada nos estudos entre padrão alimentar e fatores de risco cardiometabólicos em crianças e adolescentes.
Fonte dos dadosEste artigo seguiu as recomendações do PRISMA, que objetiva orientar as publicações de revisão na área da saúde. A estratégia de busca dos artigos incluiu pesquisas nas bases eletrônicas Medline via PubMed, Scopus e Lilacs. Não houve data limite de publicação. Os descritores foram usados em inglês de acordo com MeSH e em português segundo os DeCS. Apenas artigos de padrão alimentar extraídos pela metodologia a posteriori foram incluídos. A pergunta a ser respondida foi: quanto um padrão alimentar “não saudável” pode influenciar nos marcadores bioquímicos e inflamatórios dessa população.
Síntese dos dadosOs estudos demonstraram haver associação entre os padrões alimentares e alterações cardiometabólicas. Os padrões caracterizados como não saudáveis eram marcados pelo consumo de produtos ultraprocessados, pobres em fibras e ricos em sódio, gordura e carboidratos refinados. Apesar das associações, em vários estudos, a força dessa associação para alguns marcadores de risco era reduzida ou perdida após os ajustes para as variáveis de confusão.
ConclusãoHouve associação positiva entre os padrões alimentares “não saudáveis” e as alterações cardiometabólicas em crianças e adolescentes. Algumas associações não confirmadas podem estar relacionadas a própria dificuldade de avaliar o consumo alimentar. Apesar disso, estudos envolvendo padrões alimentares e sua associação a fatores de risco devem ser realizados em crianças e adolescentes objetivando intervenções e modificações precoces nos hábitos alimentares tidos como não adequados.
Overweight in childhood and adolescence is a major concern worldwide.1,2 Little is known about the complications that early-onset obesity can cause in the long term.3,4 Given the uncertainties, many associations have been made to better understand the consequences of overweight and obesity for the onset of cardiometabolic complications in early life.1,5
Some established associations between the genesis of obesity and alterations in cardiovascular risk markers – such as inflammatory cytokines, C-reactive protein, traditional biochemical parameters (total cholesterol, triglycerides, glucose, insulin), diet, and physical activity – have been evaluated in studies with adults and much is already known about the direction of these relations.4,6 However, it can be observed that these studies are not very common in children and adolescents, and more consistent information is still necessary about the behavior of cardiometabolic and inflammatory risk factors in this period.3,5
Diet is an important modifiable risk factor in the etiology of diseases, given the increasing number of epidemiological studies that address its relation with the onset of chronic diseases.7–9 The methodology of identification of the dietary pattern of specific populations has been widely used in observational studies, and has been useful to identify the association between diet and cardiometabolic risk factors.8,10,11
Dietary patterns can better inform about diet-disease associations than the assessment of isolated foods or nutrients, because they consider the total dietary intake and the interrelationships between many foods and nutrients, as well as their synergistic effects.7,9 They have been widely used due to the understanding that nutrients are rarely consumed in isolation, and that nutrient-only investigations underestimate the possible interactions between nutrients or between foods and other diet components.8
The identification of dietary patterns considered to be unhealthy may be related to changes in body composition and biochemical and inflammatory parameters in children and adolescents.7,10 Considering that childhood is a phase during which eating habits are formed, the adoption of healthy eating practices in this period can have favorable consequences for the rest of life.
In this sense, the aim of this systematic review article was to evaluate the association found between dietary patterns and cardiometabolic risk factors in studies of children and adolescents. The hypothesis was that unhealthy dietary patterns are associated with alterations in these risk markers in the assessed group.
MethodsThe systematic review was carried out according to the recommendations of Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA), which aims to guide systematic reviews and meta-analyses in the health area.12 The article search strategy included searches in the electronic databases MEDLINE (National Library of Medicine, USA) via PubMed, Scopus, LILACS (Latin American and Caribbean Literature in Health Sciences), and SciELO (Scientific Electronic Library Online), with no publication date limitations.
Article identification and selection in all databases were simultaneously performed by two researchers during a three-month period between February and April 2016. The words used as descriptors were: diet, dietary, patterns, risk, cardiovascular, biomarkers, children, adolescent, and health. The descriptors were used in English according to the Medical Subject Headings (MeSH) and in Portuguese according to the Descriptors in Health Sciences (in Portuguese, Descritores em Ciências da Saúde [DeCS]).
The searches in the databases were performed using the keywords with Boolean operators represented by the connector terms AND, OR, and NOT. Thus, the following combinations were used: dietary patterns AND risk AND cardiovascular AND adolescent; dietary patterns AND risk AND cardiovascular AND children; dietary patterns AND biomarkers AND cardiovascular AND adolescent; dietary patterns AND biomarkers AND cardiovascular AND children; dietary patterns AND health AND cardiovascular AND adolescent; dietary patterns AND health AND cardiovascular AND children; diet AND risk AND cardiovascular AND adolescent; diet AND risk AND cardiovascular AND children. These combinations were also used for the terms OR and NOT, respectively, in all searched databases.
The review searched for studies that evaluated dietary patterns using the a posteriori methodology only, which uses multivariate analysis techniques to extract the patterns,13 and that associated the pattern found with cardiometabolic risk factors in children and/or adolescents. The articles that considered only food pattern identification or that only associated the pattern with anthropometric measurements were not included, as the objective was to detect how much a food pattern classified as “unhealthy” could influence the biochemical and inflammatory markers in this population.
As non-inclusion criteria, the authors highlight studies conducted with adults, pregnant women, children under 2 years of age, review articles, experts’ comments, and those published in languages other than Portuguese and English.
Article selection and identification in the databases were independently and systematically performed by two researchers, who carried out the initial identification through the titles of the publications found by the descriptors and, later, by the abstracts obtained by electronic search. After the selection of publications by titles and abstracts, a new assessment was made by the two researchers, who consensually determined the studies to be read in full and included in the review. The references of the selected studies were assessed, aiming to include other articles of potential interest.
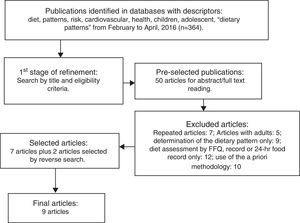
ResultsA total of 364 articles were identified on this topic. Of the 50 publications selected for reading of the abstract and of the full text, only seven articles met the established criteria for this systematic review, and two were found through the references of the first selected articles (Fig. 1).
The main characteristics of the studies, such as location, year of publication, design, age of the participants, statistical analysis used for food pattern derivation, and the other assessed variables, are described in Table 1. The articles differ regarding the type of design and in terms of the sample age, with most (78%) being cross-sectional studies.
Characteristics of the evaluated studies.
| Author/year | Country | Design | Age (n) | Reference method | Statistical analysisa | Anthropometry | Tests |
|---|---|---|---|---|---|---|---|
| Appannah et al., 201510 | Australia | Cohort | 14 (n=1611) and 17 years (n=1009) | Semi-quantitative FFQ related to previous 12 months | Reduced rank regressionb | Height, weight, BMI, WC | Insulin, glucose, TG, HDL-c, LDL-c, HOMA-ir |
| Karatzi et al., 20148 | Greece | Cross-sectional | 9–13 years (n=1912) | 24-h food record (two days a week and one weekend) | Principal component analysisc | Weight, height, WC | Insulin, glucose, HOMA-ir |
| Biblioni et al., 201316 | Spain | Cross-sectional | 12–17 years (n=219) | Validated semi-quantitative FFQ related to previous 12 months | Principal component analysis | Weight, height, WC, WtHR | Adiponectin, leptin, TNF-α, PAI-1, IL-6 |
| Park et al., 201314 | Korea | Cross-sectional | 8–9 years (n=1008) | 24-h food record (performed in three days) | Principal component analysis | WC, BMI, blood pressure | Glucose, TC, TG, HDL-c, ALT, AST and CT/HDL-c, TG/HDL-c |
| Shang et al., 201217 | China | Cross-sectional | 6–13 years (n=5267) | 24-h food record (two days a week and one weekend) | Grouping analysis | Weight, height, BMI, blood pressure, WC | Glucose, TC, TG, HDL-c, LDL-c |
| Romero-Polvo et al., 201215 | Mexico | Cross-sectional. | 7–18 years (n=916) | Semi-quantitative FFQ related to previous 12 months | Principal component analysis | Weight, height, BMI, WC, body fat% (DXA) | Glucose, insulin, HOMA-ir |
| Dishchekenian et al., 20119 | Brazil | Cross-sectional | 14–19 years (n=76) | Four-day food record (three days a week and one weekend) | Principal component analysis | Weight, height, blood pressure | TC, LDL-c, HDL-c, TG, glycemia, insulin |
| Ambrosini et al., 20107 | Australia | Cohort cross-sectional | 14 years (n=1139) | Semi-quantitative FFQ related to previous 12 months | Principal component analysis | Weight, height, WC, blood pressure | TC, LDL-c, HDL-c TG, glycemia and insulin, HOMA-ir |
| Mikkilä et al., 200718 | Finland | Cohort | 3–39 years (n=1200) | 48-h food record | Principal component analysis | Height, weight, BMI, blood pressure | CRP, TC, LDL-c, HDL-c, VLDL-c, Apo A1s, Apo B, triacylglycerol, insulin, homocysteine |
FFQ, food frequency questionnaire; BMI, body mass index; WC, waist circumference; TG, triglycerides; HDL-c, high-density lipoprotein cholesterol; LDL-c, low-density lipoprotein cholesterol; HOMA-IR, homeostasis model assessment – insulin resistance; PAI-1, plasminogen activator inhibitor-1; IL-6, interleukin 6; WtHR, waist to height ratio; TC, total cholesterol; ALT, alanine aminotransferase; AST, aspartate aminotransferase; CRP, C-reactive protein; Apo A1, apolipoprotein A1; ApoB, apolipoprotein B; DXA, dual-energy X-ray absorptiometry.
Table 2 shows the identified confounding factors that were included in the regression models, the identified food patterns named according to the definition of each author, and the main results of the articles. Confounding factors were described because they are important for the necessary adjustments in statistical analyses to increase the accuracy of the association strength. In most publications, the authors performed the analyses divided into models adjusted first for gender and age and then for other variables that could influence the characteristics of the food pattern and the association with cardiometabolic risk markers, such as parental level of schooling, level of physical activity, income, pubertal stage, and total energy intake.10,14,15
Confounding/interaction factors, identified patterns, and main results of the evaluated articles.
| Author/year | Confounding/interaction factors | Identified patterns | Main results |
|---|---|---|---|
| Appannah et al., 201510 | Physical activity, smoking status, gender, age, dietary underreporting | 1. Energetically dense. 2. High in fat. 3. Poor in fiber. | High scores on dietary patterns were associated with higher chance of belonging to the high metabolic risk group for boys (OR: 1.20, 95% CI: 1.01–1.41), but not for girls (OR: 1.03, 95% CI: 0.87–1.22) when adjusted for physical activity and smoking status. Higher scores on dietary patterns were associated with higher insulin levels (F and M-β: 3.0, 95% CI: 1–7%) and HOMA-IR (F and M-β: 4.0, 95% CI: 1–7%) in both genders. |
| Karatzi et al., 20148 | Gender, breakfast consumption, pubertal stage, waist circumference, parents’ BMI, socioeconomic status, birth weight, physical activity. | 1. Fried potatoes, red meat, and sweetened drinks. 2. Processed meats and cheese. 3. Margarine, sweets, and savory snacks. 4. Vegetables and fruits. 5. Increased egg consumption and lower consumption of fish. | The dietary pattern containing margarines, sweets, and snacks was positively associated with HOMA-IR (β=0.08; p=0.02) after adjustment for confounding factors. Children who had higher adherence to this eating pattern (consumption in the highest tertile) were 2.51 times more likely to have insulin resistance compared to children in the first tertile (95% CI: 1.30–4.90). |
| Bibiloni et al., 201316 | Age, physical activity, smoking, energy intake, BMI, WtHR. | 1. Mediterranean diet. 2. Western diet. | Western diet score was inversely related to plasma concentrations of adiponectin and IL-6 after control for possible confounding factors (β=−0.177, p<0.050 and β=0.183, p<0.050, respectively) and with additional adjustment for the BMI and WtHR (β=−0.168, p=0.050 and β=0.177, p<0.050, respectively). |
| Park et al., 201314 | Age, gender, energy intake, height, blood pressure. | 1. Balanced pattern. 2. Western pattern. | In girls, the mean concentration of triglycerides decreased in the highest consumption quintile of the balanced pattern (mean: 72.6, SD: 8.27, p=0.032). The highest score in the Western pattern was present in the girls who had more than one risk factor for MS (mean: 29.5, SD: 1.37, p=0.026). No association was found for the male gender. |
| Shang et al., 201217 | Gender, age, birth weight, eating profile in the 4th month after birth, total energy intake, physical activity, parents’ weight, level of schooling, income. | 1. Healthy dietary pattern. 2. Transition pattern. 3. Western pattern. | The fasting glucose level was higher in the western food pattern than in the healthy pattern (4.53mmol/L vs. 4.46mmol/L, p=0.0082). Children with the Western pattern had higher concentrations of LDL-c (2.156mmol/L vs. 2.07mmol/L, p=0.0023) and lower HDL-c concentrations (p<0.001) compared to those with the healthy pattern. Children with the Western pattern profile were 1.80 times (95% CI: 1.15– 2.81) more likely to be obese than those with the healthy pattern. Transition (OR: 1.31, 95% CI: 1.09–1.56) and Western (OR: 1.71, 95% CI: 1.13–2.56) food patterns were associated with abdominal obesity. |
| Romero-Polvo et al., 201215 | Gender, age, sexual maturation, BMI, physical activity, screen time, energy intake, use of medication, supplements, multivitamins. | 1. Western pattern. 2. Prudent pattern. 3. High protein/fat consumption pattern. | Insulin resistance was associated with the highest consumption quintiles of the Western dietary pattern (OR: 1.92; 95% CI: 1.08–3.43). The other identified patterns showed no significant association. |
| Dishchekenian et al., 20119 | Gender, age, ethnicity, income, maternal schooling, BMI. | 1. Traditional pattern. 2. Transition pattern 3. Fast food pattern. | The traditional pattern had a positive association with insulin (β=0.156, p<0.001), glycemia (β=0.329, p=0.027), and TG (β=0.513, p<0.001), and negative association with HDL-=−0.297; p=0.020) after adjusting for confounding factors. The fast food pattern was associated with insulin (β=0.176; p<0.001) when adjusted only by gender and ethnicity. When adjusted by income, maternal education, and BMI, this pattern showed a positive association with LDL-c (β=0.334, p<0.001), SBP (β=0.469, p<0.001), and DBP (β=0.615, p<0.001), and a negative one with HDL-c (β: −0.250, p<0.001). |
| Ambrosini et al., 20107 | Gender, energy intake, physical activity, screen time, maternal schooling, parents’ marital status, BMI, WC. | 1. Western pattern. 2. Healthy pattern. | The mean BMI and WC did not vary according to the quartiles for each dietary pattern. For girls, the chances of metabolic risk were approximately 2.5 times higher (p<0.05; 95% CI: 1.05–5.98) in the highest quartile of the “Western” food pattern when compared to the lowest. |
| Mikkilä et al., 200718 | Age, smoking status, total energy consumption, smoking, physical activity, years of follow-up in the study. | 1. Traditional pattern. 2. Health-conscious pattern. | The health-conscious pattern was associated with lower risk factors, but mainly among females. The levels of TC (β: −0.06, p=0.02), LDL-c (β: −0.07, p=0.01), Apo B (β: −0.07, p=0.03), and CRP (β: −0.09;=0.04) showed a negative association with the score of the health-conscious pattern in females, all affected by the BMI insertion in the final model. Additionally, the score of the health-conscious pattern showed an independent inverse association with homocysteine levels (F-β: −0.11, p=0.03 and M-β: −0.14; p<0.01) in both genders. |
OR, odds ratio; β, regression coefficient β; 95% CI, 95% confidence interval; F, female; M, male; BMI, body mass index; WC, waist circumference; HOMA-IR, homeostasis model assessment – insulin resistance; WtHR, waist to height ratio; TC, total cholesterol; LDL-c, low-density lipoprotein cholesterol; Apo B, apolipoprotein B; CRP, C-reactive protein; TG, triglycerides; HDL-c, high-density lipoprotein cholesterol; SBP, systolic blood pressure; DBP, diastolic blood pressure.
During the reading of the articles, the authors described the difficulty of approaching the association between dietary patterns and cardiometabolic risk factors in the group of children and adolescents, since there is little information available on the effects of dietary patterns on cardiometabolic alterations in the pediatric group.9,10,16 However, it is important to evaluate the association between dietary patterns and chronic noncommunicable diseases in childhood and adolescence, since cardiometabolic alterations can influence the current and future health of this group.17
The identification of the food pattern varied little in relation to the statistical analysis used. Principal component analysis (PCA) was the most predominant (78%), which represents an alternative approach for the evaluation of food and nutrient intake, being useful to assess the diet-disease association.7 Unhealthy eating patterns were defined as “Western” by most studies (55%), also using the terms “fast food,”9 “high consumption of protein and fat,”15 and “high in fat.”10 Only one study did not name the identified patterns, maintaining only the names of the foods that belonged to each group.8
In the methodology of four studies, parents or guardians assisted in the evaluation of children's food consumption.10,14,15,18 In 2013, Park et al.14 performed the dietary assessment in a subgroup of their sample (503 participants); the authors explained that this practice was adopted due to practical difficulties in collecting the data.
In general, a positive association was observed in the studies between an “unhealthy” eating pattern and increased cardiometabolic risk.7–10,14–18
According to Apannah et al., in 2015,10 the pattern identified as energetically dense, high in fat, and low in fiber was associated with cardiometabolic alterations, such as high insulin concentration and insulin resistance in both genders. In contrast, Karatzi et al., in 20148 found that, of the five identified food patterns, only the pattern characterized by “margarine, sweets, and snacks” was associated with insulin resistance after the adjustments for confounding factors.
Bibiloni et al.,16 in a 2013 study with 219 girls aged 12–19, identified that the Western dietary pattern was associated with a higher concentration of adiponectin and interleukin-6 (IL-6). However, the authors observed that inflammation was more influenced by body mass index (BMI) and waist-to-height ratio (WtHR) than by the identified food pattern.
Park et al.,14 in a 2013 study with Korean prepubertal children, identified two eating patterns (“balanced” and “Western”), and found no association with metabolic alterations in boys. In girls, the mean concentration of triglycerides decreased at the highest quintile of the balanced pattern of consumption (mean: 72.6, SD: 8.27, p=0.032). The “Western” pattern showed a higher score in the category with more than one risk factor for metabolic syndrome (MS) in the group of girls (mean: 29.5, SD: 1.37, p=0.026).
In 2013, Shang et al.,17 when evaluating 5267 children and adolescents aged 6–13 years of age, found that the “Western pattern” was associated with a higher chance of obesity and that children and adolescents with higher scores in the “Western” and “transition” patterns had a higher chance of abdominal obesity. There was no association between the identified dietary patterns and hypertension, hypertriglyceridemia, hypercholesterolemia, dyslipidemia, and MS. However, the “Western” pattern had higher mean values of weight, BMI, waist circumference, and systolic and diastolic pressure, and higher concentrations of glucose, LDL-c, and triglycerides, and was inversely associated with HDL-c concentration when compared to the “healthy” pattern.
In 2012, Romero-Polvo et al.15 found that children and adolescents with “Western” food patterns had a 1.92-fold higher chance of insulin resistance. In 2011, Dishchekenian et al.9 found a positive association between the “transition” pattern, based predominantly on the consumption of rice, pasta, beans, oil, red meats, processed meats, and sweets, and increased concentrations of insulin, glucose, triglycerides, and diastolic blood pressure levels. In the “fast food” pattern, the authors found a positive association with the concentration of LDL-c, and systolic and diastolic blood pressure levels, and a negative association with HDL-c.
In 2010, Ambrosini et al.,7 when studying the components of the metabolic syndrome (MS) in adolescents, divided their sample into two groups: high metabolic risk and low metabolic risk, aiming to investigate the association between dietary pattern and risk markers for MS and cardiovascular disease. The authors observed that the “Western” pattern was associated with increased risk of metabolic syndrome and its increased components, such as total serum cholesterol, BMI, and waist circumference among female adolescents. The “healthy” dietary pattern was associated with lower glucose concentrations in male and female adolescents.
In 2007, Mikkilä et al.,18 when evaluating the food intake of children and adolescents in a cohort study, identified the “traditional” and “health-conscious” dietary patterns. The second dietary pattern was inversely associated with cardiovascular risk factors; however, the results suggest that this dietary pattern is more of an indicator of an overall healthy lifestyle than just adequate dietary choices.
DiscussionThe results of the studies showed a positive association between unhealthy eating patterns and cardiometabolic alterations.7–10,14–18 However, it is important to understand that, in several studies, the strength of this association for some risk markers was reduced, while others lost it after the adjustments for confounding factors or interaction variables.7,9,10,14–17
These results are noteworthy, as several factors associated with dietary intake and cardiometabolic alterations – such as income, gender, age, birth weight, parental level of schooling, physical activity level, and food availability at home – may alter the association between diet and disease, being of the utmost importance to evaluate them.
The inability to identify positive associations between some risk factors and unhealthy foods in cross-sectional studies may be partly explained by changes in eating habits or dietary restrictions when body composition alterations already exist in children/adolescents, such as overweight and obesity, known as reverse causality.11,19 Another inability to identify positive associations is the fact that estimating true dietary intake is often complicated, as underreporting may occur in records, when the information is forgotten. This inaccuracy makes it difficult to analyze energy and macro- and micronutrient intake, as well as their associations with cardiometabolic alterations.20
Most of the studies identified the pattern characterized as unhealthy, consisting of the consumption of ultraprocessed foods, poor in fiber and rich in sodium, fat, and refined carbohydrates.7–10,14–18
It is observed that the high consumption of foods with higher energetic density, rich in fats and refined sugars, is directly associated to the increase of lipogenesis, the secretion of very low density lipoproteins, and the reduced oxidation and greater accumulation of fatty acids in the tissues and blood.21 The substitution of traditional and healthy food consumption by ultraprocessed and ready-to-eat foods and beverages is associated with the increase in the prevalence of overweight and chronic diseases already present in pediatric patients.22,23 In contrast, adequate consumption of healthy foods helps to reduce nutritional deficiencies and contributes to the maintenance of body weight and the prevention of chronic diseases,24 thus it is essential to stimulate children and adolescents not only regarding the daily consumption of adequate foods, but also the reduction in the consumption of ultraprocessed foods.
The articles selected for this review were those that addressed only the a posteriori methodology. This, in turn, consists in an exploratory method that uses multivariate analysis techniques to extract dietary patterns. In this approach, the most relevant patterns of the assessed population are identified from correlations between the collected data in the food surveys.13,25 This food consumption assessment methodology allows addressing the interactions between nutrients, food, and other diet components.
Dietary patterns offer a new approach in nutritional epidemiology, with results that can be more easily translated into advice for the population, since food-orientated guidelines are more easily interpreted and practiced by the population than nutrient-related ones.18
Despite the importance of studies with dietary patterns, few studies were performed with children and adolescents. Some difficulties are reported, such as the need to evaluate food intake in the presence of parents and the fact that the diseases are not yet established at this stage, which decreases the interest in investigating healthy populations.5,10,25 Additionally, many cardiometabolic risk factors that can be used to verify associations between diet and disease do not have established cutoffs for children and adolescents.5,6,26 This is what occurs with the definition of metabolic syndrome, which does not have well-established criteria to date and, therefore, it is difficult to assess its real prevalence in the pediatric population.14,27
It can be observed that some risk markers widely used in adults are still not frequently assessed in children and adolescents, as is the case of C-reactive protein, thus it is necessary to define cutoffs and their association with cardiometabolic alterations in the early stages of life.5
There are also limitations related to the investigation of food consumption in relation to the methods used, the lack of tool validation, food composition tables that frequently do not include the analyzed foods, diversity in the composition of industrialized products, the interviewees’ difficulty in measuring food and beverage portions, as well as underreporting of the data.9,28
Irrespective of the complexity of this association, assessments of dietary patterns and other cardiometabolic risk factors in children and adolescents should be performed, since this population is easily influenced by the environment in which they live, by food advertisers, by peers, family, and by the adopted sociocultural values.9,17,29 Recognizing that the prevalence of overweight and obesity is increasing in developed and developing countries, and that this increase in overweight has raised the economic costs of countries and the families affected by the problem, information on food consumption and changes in cardiometabolic risk factors should always be evaluated.2,17,30
Some studies have described that childhood obesity can induce early changes in metabolism, leading to dyslipidemia and glucose intolerance, in parallel with changes in the oxidative and inflammatory system, as well as the early onset of obesity, which may determine a more severe pro-inflammatory phenotype than the adult obesity.4,27,31
In 2013, Bibiloni et al.16 reported that the inflammatory process exists in the adipose tissue of obese children, representing an early alteration in humans. From this perspective, the identification and prevention, preferably in childhood, of risk factors associated with cardiometabolic alterations may be the best strategy to prevent the progression and involvement of other undesirable health effects.2
Because diet is one of the modifiable and important risk factors in the etiology of chronic diseases, the identification of eating patterns characterized by consumption of “unhealthy” foods in childhood and adolescence can be useful for the development of strategies that improve eating habits and, consequently, reduce the prevalence of these risk factors throughout life.7
The authors report that dietary patterns are specific to particular populations, since they may vary with gender, age, culture, ethnicity, socioeconomic status, and food availability, and it is important to analyze them in different groups to verify their actual applicability.9,11
The specificity of the population regarding the type of consumed dietary pattern, related to sociocultural characteristics, causes difficulties in comparisons, even though some similarities can be observed.11,18 Therefore, caution should be exercised when comparing the studies, since many of them differ in terms of sample size, number of follow-ups, statistical methods, and food consumption assessment methods.32
ConclusionThere was a positive association between “unhealthy” dietary patterns and cardiometabolic alterations by most studies with children and adolescents. Some associations that could not be confirmed may be related to the specific difficulty of evaluating food consumption. Some points should be considered in assessing the diet-disease association, such as limitations of the selected dietary survey, incomplete food composition tables, under-notifications due to omissions or forgetfulness, and even the need for parental or caregiver assistance to provide the information.
Given the complexity of this association, it is important to evaluate the dietary patterns in different populations of interest, since they may vary according to gender, age, availability of food at home, and sociocultural differences, among others. As similar as the results may seem, the comparisons and extrapolations of the data to other populations are uncertain.
Studies with dietary patterns and their associations with cardiometabolic risk factors should be performed in children and adolescents, since the prevalence of obesity and associated comorbidities is increasing in this population, so that early interventions can be performed with the objective of reducing short-and-long term health damage, as well as the reduction of costs involved in the care of health complications.
Conflicts of interestThe authors declare no conflicts of interest.
Please cite this article as: Rocha NP, Milagres LC, Longo GZ, Ribeiro AQ, Novaes JF. Association between dietary pattern and cardiometabolic risk in children and adolescents: a systematic review. J Pediatr (Rio J). 2017;93:214–22.