To identify and characterize hospital admissions and readmissions in the Brazilian Unified Public Health System (Sistema Único de Saúde [SUS]) in children with sickle cell disease diagnosed by the Minas Gerais Newborn Screening Program between 1999 and 2012.
MethodsHospital Admission Authorizations with the D57 (International Classification of Diseases-10) code in the fields of primary or secondary diagnosis were retrieved from the SUS Databank (1999–2012). There were 2991 hospitalizations for 969 children.
Results73.2% of children had hemoglobin SS/Sβ0-thalassemia and 48% were girls. The mean age was 4.3±3.2 years, the mean number of hospitalizations, 3.1±3.3, and the hospital length of stay, 5±3.9 days. Hospital readmissions occurred for 16.7% of children; 10% of admissions were associated with readmission within 30 days after discharge; 33% of readmissions occurred within seven days post-discharge. There were 41 deaths, 95% of which were in-hospital. Secondary diagnoses were not recorded in 96% of admissions, making it impossible to know the reason for admission. In 62% of cases, hospitalizations occurred in the child's county of residence. The total number of hospitalizations of children under 14 with sickle cell disease relative to the total of pediatric hospitalizations increased from 0.12% in 1999 to 0.37% in 2012.
ConclusionsA high demand for hospital care in children with sickle cell disease was evident. The number of hospitalizations increased from 1999 to 2012, suggesting that the disease has become more “visible.” Knowledge of the characteristics of these admissions can help in the planning of care for these children in the SUS.
Identificar e caracterizar as internações e reinternações hospitalares no Sistema Único de Saúde (SUS) de crianças com doença falciforme, diagnosticadas pelo Programa de Triagem Neonatal de Minas Gerais entre 1999 e 2012.
MétodosExtraíram-se do banco de dados do SUS as Autorizações de Internação Hospitalar com o código D57 (Classificação Internacional de Doenças10) nos campos de diagnóstico primário ou secundário (1999-2012). Identificaram-se 969 crianças, totalizando 2.991 internações.
Resultados73,2% das crianças tinham hemoglobina SS/Sβ0- talassemia e 48% eram meninas. A média de idade foi de 4,3±3,2 anos, a do número de internações, 3,1±3,3 e a do tempo de permanência, 5±3,9 dias. As readmissões hospitalares ocorreram em 16,7% das crianças; 10% das internações se associaram à readmissão em até 30 dias pós-alta; 33% das readmissões ocorreram em até 7 dias pós-alta. Ocorreram 41 óbitos, 95% em ambiente hospitalar. O diagnóstico secundário não foi registrado em 96% das internações, impossibilitando conhecer o motivo da internação. Em 62% dos casos, as internações ocorreram no município de residência da criança. O total de internações de crianças até 14 anos com doença falciforme em relação ao total das internações pediátricas passou de 0,12% em 1999 para 0,37% em 2012.
ConclusõesConstatou-se elevada demanda por cuidados hospitalares, cujo aumento relativo entre 1999 e 2012 sugere incremento da “visibilidade” da doença falciforme. O conhecimento das características dessas internações pode contribuir no planejamento do cuidado na rede assistencial do SUS.
According to the World Health Organization (WHO) publications, it is believed that 270million people worldwide (7% of the world's population) carry genes that determine the presence of abnormal hemoglobins (Hb).1–3 Sickle cell disease (SCD) is a genetic disorder of great clinical and epidemiological importance, whose basic etiology is the inheritance of the beta S-globin gene, either in the homozygous state or combined with another mutant allele that pathologically interacts with hemoglobin S. In Brazil, the number of people with SCD is estimated at 25,000–30,000 and the number of newborns is estimated at 3500 a year.4 According to the Neonatal Screening Program of the state of Minas Gerais (PTN-MG), the incidence of the sickle cell trait is 3.3% in a total of approximately 250,000 newborns a year; the SCD rate is approximately 1:1400.5
The onset of the disease's clinical manifestations usually occurs after the age of 3 months and lasts throughout life, with a marked variation in severity between the affected individuals. They can be grouped according to two basic pathophysiological events: vasoconstriction and chronic hemolysis.6–8 Clinical events such as painful crises,9 bacterial infections, acute chest syndrome, and chronic complications lead to several hospital admissions and high morbidity. Although most of the health problems of individuals with SCD can be cared for in primary care services, some acute events, including severe vaso-occlusive crises, require repeated hospital admissions.10
There are few national bibliographical references on the epidemiological aspects of hospital admissions by SCD. The aim of this study was to describe the hospital admissions of children with SCD that were screened by the State Neonatal Screening Program, in hospital units of the Brazilian Unified Health System (SUS), in Minas Gerais, based on information contained in the database of the SUS Hospital Information System (SIH). Associations between hospital admissions and clinical and epidemiological variables were also investigated.
MethodsThe descriptive and cross-sectional study was based on secondary data from the hospital admission system (SIH-SUS) for the state of Minas Gerais. Data related to all children screened for SCD by the PTN-MG, born between 01/01/1999 and 12/31/2012, were surveyed in the SIH-SUS.
The PMN-MG database contains data on all the 853 municipalities of Minas Gerais enrolled in the program. The coverage is approximately 92% of newborns in the state; the rest are screened by private laboratories. Between 1999 and 2012, the PTN-MG screened 3,590,315 children. Of these, 2560 were positive for SCD and referred for follow-up at the Blood Centers of the Hemominas Foundation.
The SIH-SUS is managed by the Ministry of Health and processed by DATASUS – the Department of Informatics of SUS. SUS hospital units throughout Brazil send the information on hospitalizations through the Hospital Admission Authorization (AIH). These data (approximately 50 variables) are processed by DATASUS, generating the financial credits related to the provided services.
Data from hospitalizations related to the morbidity group code D57 (Sickle cell Disorders) of the International Code of Diseases, version 10 (ICD-10) recorded in the primary and/or secondary diagnostic fields of the AIH form in the study period, were obtained after formalized request to the Brazilian Ministry of Health, guaranteeing the confidentiality and anonymity of the patients. To identify the children screened in the SIH, data such as name, date of birth, city of residence, and mother's name were also included in the PTN-MG database.
All children with codes D57.0 (sickle cell anemia with crisis), D57.1 (sickle cell disease without crisis), D57.2 (double heterozygous disorders) or D57.8 (other sickle cell disorders) in the primary or secondary diagnosis field were included. Patients with a birth date outside the study period were excluded from the SIH database, as well as those that were not included in the PTN-MG database with a diagnosis of SCD at the screening and those with the code D57.3 (sickle cell trait). Data related to genotype and deaths were extracted from the PTN-MG database.
The analyzed variables were gender, age, hospital length of stay, genotype, number of hospitalizations, readmissions, place of residence, place of hospitalization, month of hospitalization, and hospital costs. Association between nominal variables was tested with the chi-squared or Fisher's exact test. The comparison between continuous variables with normal distribution was performed through analysis of variance and the post hoc Bonferroni test, when more than two groups were involved. Variables with non-Gaussian distribution were compared using the Kruskal–Wallis test. For all the tests, an alpha error probability ≤0.05 was considered.
The study was approved by the Ethics Committee of Universidade Federal de Minas Gerais and by the Department of Pediatrics of UFMG, without the need to sign an informed consent. The Ministry of Health authorized, after due justification, the provision of data by SIH-DATASUS.
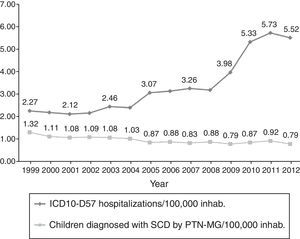
ResultsDuring the study period, 9020 hospitalizations of adults and children with ICD10-D57 (Sickle cell Disorders) were processed by DATASUS as the primary (n=8779) or secondary (n=241) diagnosis. In 2012, the hospitalizations accounted for 0.4% of all admissions through SUS, 2.4 times the percentage verified in 1999 (0.17%), excluding obstetric admissions. Fig. 1 shows the rate of children screened with SCD and the hospitalization rate of patients with ICD10-D57 registry in AIHs per 100,000 residents in Minas Gerais. The same 2.4-fold increase in the hospitalization rate is observed.
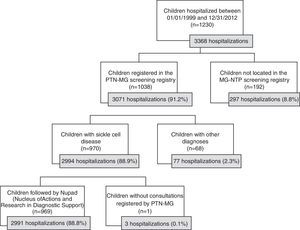
Of the aforementioned number of 9020 hospital admissions, 3368 were selected, related to children born between 01/01/1999 and 12/31/2012. Fig. 2 illustrates how the number of 2991 hospitalizations was obtained, corresponding to 969 children who comprised the study sample.
Table 1 shows the clinical and demographic characteristics of 969 children and 2991 hospitalizations. Most children had HbSS and an even higher percentage corresponded to hospitalizations of children with HbSS. Median age at the hospital admissions was 4 years. The median number of hospitalizations per patient was two (interquartile range: 1–4). The median length of hospital stay was four days. Code D57.0 (sickle cell anemia with crisis) was the one most frequently recorded in the AIHs.
Characteristics of SUS hospitalizations with code D57, from January 1999 to December 2012, of the screened children with sickle cell disease, born between January 1999 and December 2012.
| Hospitalizations (n=2991) | n % | Patients (n=969) | n % | |
|---|---|---|---|---|
| Gender | ||||
| Female | 1412 | 47.2% | 465 | 48.0% |
| Male | 1579 | 52.8% | 504 | 52.0% |
| Genotype | ||||
| Hb SS or Hb Sß0 tal | 2438 | 81.5% | 709 | 73.2% |
| Hb SC | 484 | 16.2% | 234 | 24.1% |
| Hb Sß+ tala | 66 | 2.2% | 25 | 2.6% |
| Hb SDPunjaba | 3 | 0.1% | 1 | 0.1% |
| Diagnosis of ICD-10 D57b | ||||
| D57.0 | 2296 | 76.8% | – | – |
| D57.1 | 572 | 19.1% | ||
| D57.2 | 4 | 0.1% | – | – |
| D57.3c | 4 | 0.1% | – | – |
| D57.8 | 115 | 3.8% | – | – |
Hb SS, homozygous inheritance for Hb S; Hb SDPunjab, association between Hb S and the hemoglobin variants D-Punjab; Hb SC, association between Hb S and C.
The number of children with Hb Sß+ tal and Hb SDPunjab may be overestimated, as molecular biology methods for diagnostic confirmation were introduced in the PTN-MG only in 2010.
The percentage of hospitalizations among children with SCD aged 0–14 years in relation to the total number of pediatric hospitalizations in the SUS in the same age group (SIH-SUS data) increased approximately three-fold in the study period, from 0.12% in 1999 to 0.37% in 2012.
When comparing hospital admissions for SCD with hospital admissions for other chronic diseases in the age group 0–14 years (data from the SIH-SUS), it is observed that the frequency of hospitalizations for SCD during the period increased three-fold, being similar to the frequency of admissions for cerebral palsy and diabetes mellitus in 2012.
The frequency of hospitalizations per patient is shown in Table 2. Note that 26.9% of the patients with four or more hospitalizations were responsible for 62.6% of hospital admissions. The 2–4 and 5–9 year groups showed not only a higher numbers of hospitalizations, but also a higher mean of hospitalizations per patient.
In total, 162 patients (16.7%) underwent hospital readmission within 30 days during the study period. Most of them had only one readmission (63%) and the remainder from two to seven. The mean interval between hospitalizations was 13.3±9.4 days, with one-third of readmissions occurring within seven days after hospital discharge. They were more frequent in children with SS/Sβ0tal (p<0.05).
The mean length of hospital stay was 5.0±3.92 days, ranging from 0 to 63 days. This mean length of hospital stay for pediatric hospitalizations through SUS for other causes was 5.95 days. In almost 70% of hospitalizations, the length of stay ranged from zero to five days; in only 0.9% of cases was it longer than 20 days. A higher proportion of patients with SS/Sß0 thalassemia genotype had a length of stay longer than five days (p=0.009). There was a tendency toward an increase in length of stay with age, with patients aged ≥10 years showing a higher proportion of hospitalizations lasting more than five days (p=0.035). The distribution of hospitalizations throughout the year was relatively uniform, with no seasonality observed.
The amounts spent on hospital care, recorded by SIH-SUS in US dollars, were recorded in 2444 AIHs (81.7%); in the remaining 561, the data was missing. The mean cost per hospitalization, considering the seven years for which the data were available, was 174 dollars. Considering the periods of 2005–2007 and 2010–2012, the mean annual cost of hospitalization was slightly higher in the second studied period.
According to the PTN-MG, 41 deaths occurred among the 969 children selected for the study (4.2%), most of them (n=34) with the Hb SS/Sß0tal profile. In 95% of the cases (n=39), the death occurred in the hospital environment, according to a copy of the death certificate obtained through the PTN-MG. Infection, acute chest syndrome, and splenic sequestration were the main causes of death, as disclosed by the death certificates. However, only seven deaths were recorded in the AIHs with the ICD10-D57 code in the primary and secondary diagnostic fields. In one case, the date of hospital discharge coincided with the date of death recorded by the PTN-MG, despite the fact that the death was not recorded in the AIH. The other 31 deaths recorded as hospital deaths by the PTN-MG may have occurred during hospitalizations without the registration of the ICD10-D57 code, or in emergency care units not recognized as such by PTN-MG records.
In 96% of the AIHs there was no record of another diagnosis associated to the D57 code, which made it impossible to study the comorbidities present in the hospitalizations. Infections were recorded in 90 of the 118 AIHs that contained any other diagnosis rather than the D57 group registry.
Hospitalizations occurred in 149 municipalities of Minas Gerais. The hospitalized children lived in 278 municipalities, three of which were located in other states – Verdejante (PE), Três Rios (RJ), and Novo Horizonte (BA). The municipality where the care was provided coincided with the municipality of residence in 62.1% of the cases. The city with the highest number of hospitalizations (43.5%) was the state capital, Belo Horizonte, but 54% of the hospitalized patients did not live in the capital and of the 20% who did, all received care in that city. The majority (97%) of patients living in Contagem, Ribeirão das Neves, and Santa Luzia, municipalities located in the metropolitan region, were treated in Belo Horizonte. Tabular data related to SCD comprising the prevalence, the rate of resident children, and the hospitalization rate in each of the 28 Regional Health Units of Minas Gerais can be requested from the authors.
Comparison of hospitalizations up to 4 years of life of 287 children born between 1999 and 2001 (n=129) with those born between 2006 and 2008 (n=158)A total of 696 hospitalizations found in the SIH-SUS were selected for this part of the study: 247 hospitalizations up to 4 years of life were recorded for the children born in the first period, and 449, among those born in the second period. The 129 children born in the earlier period did not differ significantly regarding gender or type of hemoglobinopathy from the 158 children born in the more recent period (p=0.35 and p=0.24, respectively).
The proportion between the number of children who had at least one hospitalization and the number of children with SCD screened by the PMN-MTN in each of the periods (623 in the first and 509 in the second) was 0.207 and 0.310, respectively, resulting in a difference of 0.103 (95% CI: 0.032–0.174, p<0.0001). The difference is even greater when the proportions between the number of hospitalizations and the number of children screened in each of the periods are calculated: 0.396 and 0.882, resulting in a difference of 0.486 (95% CI: 0.438–0.533; p<1×10−9).
The mean number of hospital admissions per child was higher in the second period when compared to the first (2.84 and 1.91, respectively, p=0.001). The hospitalization duration, however, was similar in both groups (4.57 vs. 4.64 days, respectively, p=0.85).
According to the records of 696 AIHs, there were three deaths, one of a child born in the period from 1999 to 2001 and two among those born from 2006 to 2008. However, in 88.2% of AIHs processed in the earlier period, there was no positive or negative death record (the corresponding field was blank), while all the more recently processed AIHs contained this information.
DiscussionThe most remarkable finding of the present study was that, over the years, there was a very significant increase in several parameters related to hospital admissions for SCD. In relation to the population of adults and children, a 2.4-fold increase during the assessed period was observed. If only the group aged up to 14 years is considered, the increase was the same, reaching 5.5 hospitalizations per 100,000 inhabitants in MG. Considering the age group from 0 to 14 years, the frequency of hospital admissions for SCD was similar to that for diabetes mellitus and cerebral palsy, especially among the chronic conditions that most frequently result in hospitalizations at the pediatric age range.11
This increase became more evident when the initial and final periods of the present study were compared. The number of children with at least one hospital admission and, still more evidently, the total number of admissions were much higher in the most recent period in relation to the initial one. Additionally, the frequency of admissions per child was also higher in recent years.
This absolute and relative increase could be simply explained by the increase in the frequency of hospital admissions for SCD to the detriment of other causes, resulting from changes in SCD hospital care guidelines between 1999 and 2012, which are unknown to the authors. That does not seem the most plausible reason, though. It is believed that the broader knowledge of the disease, both by the family members and by the health professionals, resulting from the initiation of the state screening program in March 1998, accounted for the more frequent registration of the D57 group codes in the AIHs. A similar phenomenon has been recently reported in the state of Maranhão.12
The discrepancy caused by the “invisibility” of SCD is also evident in a study that found the rate of hospitalization for SCD is much higher in São Paulo and Rio de Janeiro than in Bahia, where the incidence of the disease is approximately five and two-fold higher than in the other two states, respectively.3 Another indication of the disease's “invisibility” is the finding that half of the 193 children's death certificates recorded by the PTN-MG did not include the term “sickle cell.”13
The prevalence of the SS genotype in hospital admissions, as in other studies, is explained by the more severe clinical course of the disease.14,15 The most frequent cause of hospitalization, as observed in other studies,3,16–19 was the painful crisis, as code D57.0 (sickle cell anemia with crisis), which in the absence of additional data in the AIHs was interpreted by the authors as a painful crisis that required hospitalization. The mean length of stay of five days coincides with that of other studies, which observed a range of 4–11 days for hospitalizations due to vaso-occlusive crises.19–21
The regional distribution of hospitalizations followed what was expected of the hospital network concentration in MG at regional poles. In more than half of the hospitalizations in Belo Horizonte, the children lived in other municipalities, mainly in the metropolitan region. Similarly, but to a lesser extent, the same occurred in Juiz de Fora, Uberaba, and Uberlândia.
The mean cost of hospitalization in 2012 disclosed by the present study was US$ 186.00, well below the mean cost of US$ 344.6 dollars11 for pediatric hospitalizations in general, consistent with the shorter hospital length of stay, characteristic of the most frequent cause of hospital admission, the painful crisis. In a study carried out in Nigeria, the mean cost of hospitalization was US$ 133 dollars22 and, as expected, it was lower than that of the United States.23
The limitations found in the present study are associated to the quality of the data in the AIH records or, possibly, to the transfer of data recorded by the health professionals to the system database. Record failures, characterized primarily by typing errors, misinformation, or missing data, represent the most significant difficulties for searches carried out in large public databases. An extensive “database scanning” was required, compiling and cross-referencing information to reduce errors and approximate the collected data to the actual data. Nonetheless, the broad epidemiological studies on SCD based on governmental databases should be considered valid as sources of information, as after the management of these systems by diverse professionals, with different interests, it will be possible to identify failures and implement improvements.
Simple interventions and basic health care provided by more frequent follow-up at the basic health unit, in addition to that performed in blood centers and other secondary care units, prompt recognition of the warning signs for potentially severe situations, and immediate search for medical assistance may determine, over time, a lower need for hospital admissions.
In this sense, the education of the patient and his/her family, as well as of the health professionals, focusing on empowering of the knowledge about the disease and co-responsibility regarding the care and treatment are challenges to be overcome. In relation to the care network, it is necessary to train the multiprofessional team and include the information about the disease in the files of the primary care information system, to expand and improve the initial care provided by the emergency services to individuals with SCD, to include the disease in the parameters of risk regulation and classification, as well as to institute integral care of individuals with SCD within the scope of SUS.
It is expected that epidemiological research, not only in SCD, but also regarding other prevalent conditions or with a more severe evolution in the black population, be encouraged and facilitated in the institutional databases, respecting the ethical requirements of secrecy and anonymity.
The authors expect that the contributions to the knowledge on hospital admissions of children with sickle cell disease in Minas Gerais can support the planning and implementation of actions that will lead to the reduction of morbimortality determined by the disease and to the improvement of the quality of life of individuals with SCD.
FundingConselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq), Núcleo de Ações e Pesquisa em Apoio Diagnóstico (Nupad, Faculdade de Medicina da UFMG).
Conflicts of interestThe authors declare no conflicts of interest.
To Conselho Nacional de Desenvolvimento Científico e Tecnológico, for the research grant to a MBV; to José Nelio Januário, Director of Núcleo de Ações e Pesquisa em Apoio Diagnóstico (Nupad, Faculdade de Medicina da UFMG).
Please cite this article as: Fernandes AP, Avendanha FA, Viana MB. Hospitalizations of children with sickle cell disease in the Brazilian Unified Health System in the state of Minas Gerais. J Pediatr (Rio J). 2017;93:287–93.
Study carried out at Universidade Federal de Minas Gerais (UFMG), Belo Horizonte, MG, Brazil.