To evaluate the effect of maternal supplementation with vitamin E on the concentration of α-tocopherol in colostrum and its supply to the newborn.
MethodThis randomized clinical trial enrolled 99 healthy adult pregnant women; of these, 39 were assigned to the control group and 60 to the supplemented group. After an overnight fast, 5mL of blood and 2mL of colostrum were collected. After the first sampling (0h milk), the supplemented group received 400IU of supplementary vitamin E. Another 2mL milk aliquot was collected in both groups 24h after supplementation (24h milk). The samples were analyzed by high-performance liquid chromatography. The α-tocopherol content provided by colostrum was calculated by considering a daily intake of 396mL of milk and comparing the resulting value to the recommended daily intake for infants aged 0–6 months (4mg/day).
ResultsThe initial mean concentration of α-tocopherol in colostrum was 1509.3±793.7μg/dL in the control group and 1452.9±808.6μg/dL in the supplemented group. After 24h, the mean α-tocopherol concentration was 1650.6±968.7μg/dL in the control group (p>0.05) and 2346.9±1203.2μg/dL in the supplemented group (p<0.001), increasing the vitamin E supply to the newborn to 9.3mg/day. Initially, 18 women in the supplemented group provided colostrum α-tocopherol contents below 4mg/day; after supplementation only six continued to provide less than the recommended amount.
ConclusionMaternal vitamin E supplementation increases the supply of the vitamin to the infant by providing more than twice the Recommended Daily Intake.
Avaliar o efeito da suplementação materna com vitamina E sobre a concentração de α-tocoferol no colostro e o fornecimento desta para o recém-nascido.
MétodoO estudo clínico randomizado foi realizado com 99 parturientes adultas e saudáveis, sendo 39 alocadas no grupo controle e 60 no grupo suplementado. Após jejum noturno, foram coletadas 5mL de sangue e 2mL de colostro das parturientes. Após a primeira coleta (leite 0h), o grupo suplementado recebeu suplementação com 400 UI de vitamina E. Foi realizada nova coleta de 2mL de colostro, em ambos os grupos, 24h após a suplementação (leite 24h). As amostras foram analisadas por Cromatografia Líquida de Alta Eficiência. A quantidade de α-tocoferol fornecida pelo colostro foi considerada para uma ingestão diária de 396mL de leite e comparada com a Ingestão Diária Recomendada para crianças de 0 a 6 meses (4mg/dia).
ResultadosA concentração média inicial de α-tocoferol no colostro foi 1509,3±793,7μg/dL no grupo controle e 1452,9±808,6μg/dL no grupo suplementado. Após 24 horas a concentração média de α-tocoferol no grupo controle foi 1650,6±968,7μg/dL (p>0,05), já no grupo suplementado a concentração média foi 2346,9±1203,2μg/dL (p<0,001), aumentando assim a oferta de vitamina E para o recém-nascido para 9,3mg/dia. Inicialmente 18 mulheres do grupo suplementado forneciam valores inferiores a 4mg/dia de α-tocoferol em seu colostro, após suplementação apenas 6 continuaram a fornecer quantidade inferior ao recomendado.
ConclusãoA suplementação materna com vitamina E promove o aumento do fornecimento da vitamina para o recém-nascido, fornecendo mais do que o dobroda Ingestão Diária Recomendada.
Vitamin E is the generic term used to describe eight different molecules: α-, β-, γ-, and δ-tocopherol and α-, β-, γ-, and δ-tocotrienol.1 Among them, α-tocopherol is the only isomer related to nutritional needs of vitamin E. Vitamin E is considered one of the best biological antioxidants due to the protection offered to the plasma membrane and low-density lipoproteins against oxidation reactions and lipid peroxidation.2
Newborns are considered high-risk for vitamin E deficiency due to oxidative stress generated by postnatal transition from the intrauterine environment, relatively low in oxygen, to the extrauterine one, significantly richer in oxygen.3 Considering this vitamin deficiency risk, it is recommended that the α-tocopherol intake during the first six months of the infant's life be 4mg/day.4
It is known that the placental transfer of α-tocopherol from the mother to the infant is limited, even if there is an increase in maternal intake of vitamin E.5 Thus, the newborn may have low reserves of vitamin E, making it necessary that breast milk provide an adequate amount of vitamin E to ensure the formation of vitamin reserves and reinforce the newborn's defenses against oxidative stress.6
Insufficient intake of this nutrient at this stage of life (especially from the 6th to 8th week) can affect the development of the immune and pulmonary systems.7 However, if regular breastfeeding occurs, nutritional deficiency symptoms are generally not observed in children.8
Venous supplementation with high doses of vitamin E in infants increases the risk of sepsis and reduces supplementation efficiency in fighting severe retinopathy.9 Therefore, maternal supplementation to improve the nutritional status of the neonate through satisfactory amounts of α-tocopherol provided by colostrum becomes the safest way to prevent possible vitamin E deficiency, as it will be slowly released during the feedings, contributing to the formation of body reserves, since placental transfer is limited.6
Thus, the aim of this study was to investigate the effect of maternal supplementation with vitamin E on the concentration of α-tocopherol in colostrum and consequently on the supply of this vitamin for the neonate.
MethodsEthical considerationsThe study was approved by the Research Ethics Committee – REC da Universidade Federal do Rio Grande do Norte – CAAE 0260.0.051.294-11.
Study populationFor the calculation of the required minimum sample size, deductive power analysis was used, through GPower® software, version 3 (G Power®, Germany). The parameters taken into consideration were: effect size d=0.5, probability of error α=0.05, power test β=0.95, and a 95% confidence interval. Using these parameters, the minimum required sample consisted of 22 subjects for each group. A total of 99 adult and healthy pregnant women participated in this study; 39 were allocated to the control group and 60 to the supplemented group.
Sampling was carried out by convenience, comprising pregnant, female volunteers aged 18–40 years, without pathologies (diabetes, hypertension, cancer, diseases of the gastrointestinal tract, liver, heart diseases, infections, syphilis and/or HIV positive), who had delivered a full-term, single infant without malformations and did not use vitamin supplements during pregnancy.
Study designThe randomized clinical trial was carried out from January 2012 to March 2013, at the Maternity School, in Brazil. Women that met the research criteria were invited to participate in the study and signed the Free and Informed Consent (FIC).
Every mother who accepted to participate in the study was allocated to a group, i.e., the control group (CG) or the supplemented group (SG), by drawing lots, with the latter receiving capsules containing 400 international units (IU) of alpha-tocopherol. Randomization was used so that all women would have the same chance of being sorted to either of the two groups.
Blood (5mL) and colostrum milk (2mL) were collected from each participant in the morning hours after an overnight fast. The collection of milk occurred in two stages, the first (0h) at the initial contact with the mother and the second 24hours (24h) after the first collection. The mothers belonging to the supplemented group received a capsule containing 400IU of alpha tocopherol, respectively, after the first milk collection (0h).
The data related to maternal and neonatal characteristics were obtained from files.
Sample collection and preparationBlood collected by venipuncture (5mL) by nurses on duty at the maternity were placed in polypropylene tubes protected from light and transported to the laboratory under refrigeration; they were then centrifuged to remove of 1000μL of serum, then stored at −18°C.
Colostrum was obtained by manual expression of one breast, always at the end of the feeding to prevent fluctuations in fat and tocopherol content. The foremilk was discarded and 2mL were collected at time 0h and another 2mL sample after 24h. These procedures were performed by the study authors themselves. As for the supplemented women, milk samples were collected 24h after supplementation. The samples were collected in polypropylene tubes protected from the light and transported under refrigeration, then were sent to the laboratory; colostrum samples were placed in a water bath at 37°C for 15min and homogenized and then a 500μL sample was removed and stored at −18°C.
Procedures for the analysisThe technique used for extracting the tocopherol in serum was adapted from Ortega et al.10 To 2mL of serum, an equal amount of 95% ethanol was added, the mixture was stirred, and 2mL of hexane were added for three extraction steps; each of the steps was stirred and centrifuged (10min, 1073×g), and the organic phase containing hexane was separated, totaling 6mL.
The methodology adapted from Romeu-Nadal et al.11 was used for the milk. To 0.5mL of colostrum was added 0.5mL of 95% ethanol. Next, the tube was submitted to mechanical agitation for 1min and the extraction process was performed in two steps with 2mL of hexane, resulting in a 4mL extraction of the hexane phase.
Of the organic compounds obtained from both samples, 2mL were evaporated using nitrogen, and the dried extract was dissolved in 0.5mL of absolute ethanol for further analysis by High Performance Liquid Chromatography (HPLC).
The α-tocopherol concentrations were determined by HPLC in a Shimadzu® LC-20AT (Shimadzu®, USA) chromatograph, equipped with a 20μL loop injector, CBM 20A (Shimadzu®, USA) communicator, and coupled to a SPD-20A UV-VIS detector (Shimadzu®, USA), with UV detection (λmax=292nm).
The chromatographic separation was carried out in an LC Shim-Pack® CLC-ODS (Shimadzu®, USA) 4.6mm×25cm reversed phase-column. The elution was isocratic with a mobile phase, consisting of methanol/ultrapure water (Milli-Q®, Millipore Sigma®, Merck, Germany) in 97:3 (v:v) with a 1.0mL/min flow. The chromatograms were integrated using the LC Solution® program (Shimadzu®, USA).
The identification and quantification of the α-tocopherol in the samples was established by comparison of the peak retention area obtained in the chromatogram with the area of the respective SIGMA® (Sigma®, Merck, Germany) alpha-tocopherol standard. The concentration of the standard was confirmed by the specific extinction coefficient in absolute ethanol, ¿ 1%, 1cm=75.8.
Confirmation of capsule concentrationTo verify whether the capsules contained 400IU of Vitamin E, they were opened and then an aliquot of each capsule was weighed, which was placed in a polypropylene tube protected from light and added to 1mL of HPLC grade Ethanol. SIGMA® (Sigma®, Merck, Germany) α-tocopherol was similarly produced.
The identification and quantification of the α-tocopherol in the capsules were established by comparing the peak area obtained in the chromatogram with the area of the respective alpha-tocopherol SIGMA® (Sigma®, Merck, Germany) standard, as well as through the specific extinction coefficient in absolute ethanol of α-tocopherol acetate ¿ 1%, 1cm=40.
The capsules contained α-tocopherol at the concentrations stated on their labels, demonstrating the actual amount provided by the capsule.
Statistical analysisStatistica 7 software (StatSoft Inc., USA) was used for statistical analysis. Alpha-tocopherol values were expressed as mean and standard deviation. To test the differences between the means of parametric numerical data, Student's t-test was used in paired samples. Differences were considered significant at p<0.05. The association between continuous variables (concentration of nutrients in milk and serum) was determined by Pearson's correlation analysis.
Nutritional needsThe amount of α-tocopherol provided by colostrum was considered for a daily intake of 396mL of milk, related to the average production of milk during the first week after delivery of mothers that had full-term newborns and compared with the dietary reference intake (DRI) for children aged 0–6 months, the equivalent to 4mg/day.4,12
ResultsDescription of the populationA total of 99 women participated in the study, with 39 allocated to the control group and 60 to the supplemented group.
The mean age in years was 24±6, most were married or living in a stable union (65%), and the level of education was varied: 36% of women did not complete primary education, whereas only 0.9% attended college/university. Family income ranged between 1 and 4 minimum wages (81.4%). The mean number of residents in the households of pregnant women was 5.4±1.6 people, with a minimum value of 2 and maximum of 10.
Regarding obstetric variables, 53.1% of women had had another pregnancy; the main type of delivery was cesarean section (58.1%) with a mean of 39.1±1.4 weeks of gestation. Most women started the pregnancy with a normal weight (51.2%); however, there was a trend for increased weight gain totaling 46.1% of women with overweight and obesity at the end of the pregnancy.
Concentrations of α-tocopherol in serumThe mothers had a mean concentration of α-tocopherol in serum of 1066.6±287.7mg/dL and 1159.6±350mg/dL, respectively in the CG and SG, with no significant difference (p=0.41) between them. Overall, 6.1% of participants (n=6) had serum levels indicating low levels of α-tocopherol (ranging from 499.6 to 697.7mg/dL), while 3.0% (n=3) had α-tocopherol deficiency (levels<499.6mg/dL).13
Concentrations of α-tocopherol in colostrum and response to supplementationThe mothers had a mean concentration of α-tocopherol in colostrum of 1509.3±793.7 and 1452.9±808.6mg/dL respectively, in the CG and SG groups at time 0h. It was found that the concentrations of α-tocopherol were similar in all groups, with no evidence that the mean levels in the groups at 0h were different (p=0.74). This fact corroborates the homogeneity of the groups, showing that participants initially had similar α-tocopherol concentrations in colostrum.
After supplementation, the mean concentration of α-tocopherol in the mothers’ colostrum was 1650.6±968.7 and 2346.9±1203.2mg/dL in the CG and SG groups, respectively.
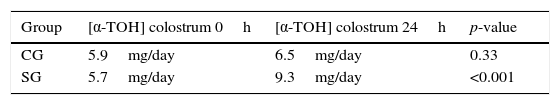
When comparing the concentrations of α-tocopherol in colostrum at times 0h and 24h, it was observed that women who did not receive supplementation (CG) showed similar concentrations at both moments (p=0.33). However, the mean α-tocopherol concentrations in supplemented women increased the concentration of α-tocopherol secreted in colostrum by 61% (p<0.001).
Newborn's nutritional needsBefore supplementation, the CG and SG groups provided amounts of α-tocopherol respectively greater than 4mg/day recommended for children aged 0–6 months (Table 1). The lowest value was 0.66mg and the highest was 14.9mg of α-tocopherol for 396mL of colostrum.
In the control group (CG), the mean α-tocopherol supply remained unchanged, as this group received no supplementation, whereas the SG group, which received the supplementation, started to provide on average 3.6mg/day more α-tocopherol for 396mL of colostrum 24h after supplementation.
When individually analyzing the women in the control group, 33% (n=13) showed values below 4mg/day of α-tocopherol in their colostrum before the supplementation, while 30% (n=18) of the supplemented group of women had the same amount of vitamin E. After supplementation, only 10% of the women (n=6) showed values below the 4mg of α-tocopherol for the newborn, while in the CG, 28% (n=11) of women still did not provide adequate amounts.
When assessing the α-tocopherol concentrations in the colostrum of supplemented women who could not provide the recommended values in their milk even after ingestion of 400IU of vitamin E, it was verified that these mothers had in common an initial concentration of α-tocopherol in colostrum lower than 2mg for 396mL.
DiscussionThe health of pregnant women and newborns depends on adequate maternal nutrition. Nutrition during pregnancy is, therefore, decisive for the gestational course and the formation of reserves for lactation. During pregnancy, symptoms such as nausea, vomiting, and heartburn may cause a reduction in food intake, especially considering that fats are not well tolerated.14 The reduction of this intake can lead to reduced consumption of α-tocopherol and, thus, it is important to verify if the mother has nutritionally adequate plasma concentrations of this vitamin.
According to Sauberlich et al.,13 the concentration of α-tocopherol in serum must be greater than or equal to 697mg/dL. Based on these reference values, the study showed an average concentration considered to be acceptable regarding α-tocopherol parameters in serum. Similar concentrations were found in the studies by Papas et al.,15 Garcia et al.,16 and Dimenstein et al.17
When individually analyzing the breastfeeding mothers, 6.1% of them had low nutritional status for α-tocopherol, a different prevalence from that in the study by de Lira et al.18 carried out at the same hospital, which found a percentage of 12% of women with α-tocopherol deficiency. This difference can be explained by the participation of adolescents in the sample group.
The concentration of α-tocopherol in 0h colostrum of the two groups was within the expected when compared to studies carried out in Brazil by Dimenstein et al.,17 who found an average concentration of α-tocopherol of 1603.4±911mg/dL, and Campos et al.,19 who found 1313.9±798.7mg/dL. Studies in the United States20 and Turkey21 showed similar results to those in this work, with α-tocopherol values in colostrum of 1335.2±198.1 and 1326.6±68.9mg/dL, respectively.
Regarding the effect of using vitamin E supplements on the increase in α-tocopherol in breast milk, studies with humans are still controversial.
Szlagatys-Sidorkiewicz et al.,22 in a study conducted in Poland, showed that the concentration of vitamin E in milk was not higher in women who received recommended vitamin supplements for pregnant and lactating women compared to those who did not (p=0.332). Also in Poland, Martysiak-Zurowska et al.23 obtained similar results, showing no correlation between dietary intake of vitamin E and the use of supplements with the concentration of alpha-tocopherol in breast milk.
However, a study in Canada found that there was a positive correlation between vitamin E found in milk and multivitamin supplementation reported by the research participants.24 In a study of the Brazilian population, Garcia et al.25 observed that 24h after vitamin E supplementation there was a significant increase in the amount of alpha-tocopherol in colostrum (p=0.04).
Based on the established reference values for α-tocopherol intake, the groups provided on average quantities >4mg/day, whereas the supplemented group showed an increase of 61.5%.
However, no one knows with certainty whether 4mg/day of α-tocopherol is sufficient at this stage of lactation, since for the determination of α-tocopherol DRI for infants aged 0–6 months, only the average intake of this nutrient was analyzed after two months of lactation.4 Thus, the first month of life has not been accounted for, a phase in which the newborn experiences an imbalance of the antioxidant system due to the transition to the extrauterine environment, which is significantly richer in oxygen.3
In addition to this increased risk of oxidative stress, it is necessary to take into account certain factors that cause variations in nutrient intake from colostrum, such as differences in the milk intake volume and concentration of nutrients during early lactation, factors that were not considered to establish the DRI, which may underestimate the neonate's real needs.
Studies on the benefits of α-tocopherol supplementation in newborns are still scarce; however, it has been reported that supplementation in the group of low birth weight infants has shown benefits that go beyond the reduction of oxidative stress. Kitajima et al.26 found that supplementation with α-tocopherol can improve mental development of infants with low birth weight, especially regarding IQ performance at school age, indicating that α-tocopherol may be an essential nutrient for mental development in childhood.
This study is in accordance with the results found by Chen et al.27 that, while assessing the levels of vitamin A, C, and E in the mother and child, found that newborn's levels of α-tocopherol were directly associated to motor, behavioral development, and developmental quotient.
However, it is known that premature infants have a higher risk of developing complications resulting from intravenous supplementation with vitamin E, such as the development of sepsis and necrotizing enterocolitis.28 Faced with this risk, it would be safer to recommend maternal supplementation of α-tocopherol, with the vitamin being transferred to the infant through breast milk. It is known that breast milk offers several benefits to the newborn, as it is a nutritionally-rich food and is free from impurities, being able to reduce morbidity and mortality and promote health benefits in the long term.29
Based on the results observed in the study, it was found that the mothers of the assessed population provided tocopherol levels above the adequate intake (AI) before supplementation; however, such supply was increased by 61.5% after supplementation.
This increase in vitamin supply was also observed by Clement et al.30 in women supplemented with vitamin E capsules in either natural or synthetic form; however, with better results than those who received RRR-α-tocopherol capsules.
In women whose α-tocopherol concentrations in breast milk were less than 4mg/day, an increase of vitamin E in milk occurred after supplementation similarly to the other mothers; however, due to the low initial levels of the vitamin, it failed to meet the infant's nutritional needs.
Maternal supplementation provides an increase in the supply of α-tocopherol, which brings benefits to the newborn, contributing to the neonate's motor and mental development,26,27 as well as strengthening the defenses against oxidative stress.6
The study shows that supplementation with 400IU of α-tocopherol in the postpartum promotes an increase in α-tocopherol concentrations in colostrum, a crucial phase for the neonate. Therefore, supplementation is recommended for women in the postpartum period, with a mega dose >400IU or daily supplementation at doses that meet the DRI, in order to meet the needs of all the mothers.
Although supplementation provides an increase in α-tocopherol levels, factors that interfere with this supplementation have not been investigated, particularly vitamin E and fat intake during pregnancy, which can be considered a study limitation. Another factor to be taken into consideration is that, because it is a cross-sectional study, it was not possible to verify the possibility of maintaining vitamin E levels during other stages of lactation.
FundingConselho Nacional de Desenvolvimento Científico e Tecnológico – CNPQ.
Conflicts of interestThe authors declare no conflicts of interest.
Please cite this article as: Melo LR, Clemente HA, Bezerra DF, Dantas RC, Ramalho HM, Dimenstein R. Effect of maternal supplementation with vitamin E on the concentration of α-tocopherol in colostrum. J Pediatr (Rio J). 2017;93:40–6.
Study carried out at Universidade Federal do Rio Grande do Norte (UFRN), Natal, RN, Brazil.